Table of Contents >> Show >> Hide
- What Shingles Usually Looks Like
- Why Shingles Is So Easy to Mistake for Something Else
- Conditions Commonly Mistaken for Shingles
- How Doctors Usually Tell the Difference
- Red Flags That Mean You Should Get Medical Care Quickly
- If It Is Shingles, What Happens Next?
- How to Lower Your Risk of Shingles
- Bottom Line: Is It Shingles or Something Else?
- Real-World Experiences: When People Wonder, “Is It Shingles or Something Else?”
Few things spark instant skin panic quite like a painful rash. One day your skin feels tingly, sensitive, or weirdly sunburned. The next day, blisters show up and your search history turns into a dermatology detective novel. Is it shingles? Poison ivy? Herpes? Eczema having a dramatic comeback tour?
The truth is that shingles can look a lot like other skin problems at first. That is why people often misread the signs, especially in the early phase before the rash fully appears. And because shingles treatment works best when started early, knowing the difference matters. A lot.
This guide breaks down what a typical shingles rash looks and feels like, which common conditions can mimic it, how doctors tell them apart, and when you should stop guessing and get checked. Think of it as a practical field guide for when your skin starts sending mixed signals.
What Shingles Usually Looks Like
Shingles, also called herpes zoster, happens when the same virus that caused chickenpox wakes up again years later. It tends to announce itself in stages. First comes the odd nerve pain: burning, tingling, stabbing, itching, or skin sensitivity in one spot. Then a rash appears, usually a few days later. After that, fluid-filled blisters show up, crust over, and gradually heal.
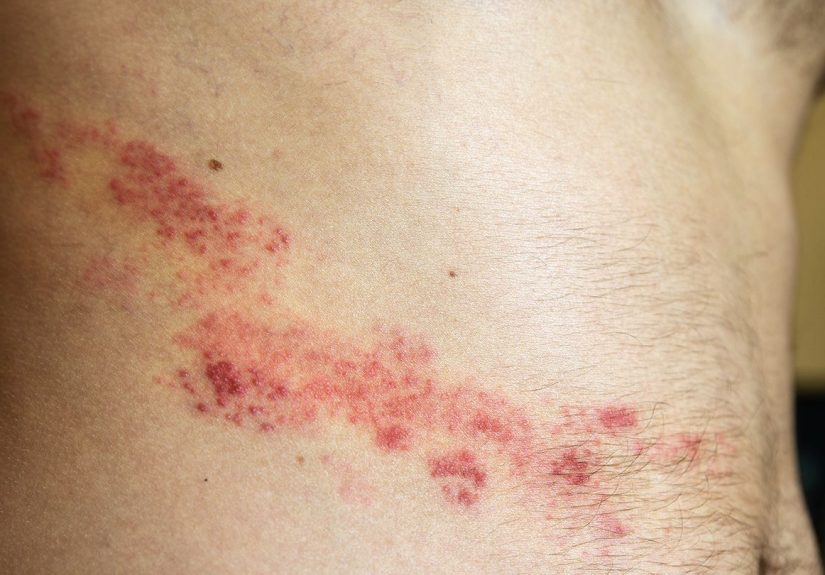
The biggest clue is the pattern. A classic shingles rash usually appears in a single stripe or band on one side of the body or face. It often wraps around the torso, but it can also show up on the neck, scalp, or one side of the face. Most cases do not cross the body’s midline. In plain English: if the rash seems to respect an invisible center line like it is following traffic laws, shingles moves higher up the suspect list.
Another clue is the pain-to-rash ratio. Shingles often hurts more than people expect. Some describe the sensation as electric, deep, or out of proportion to what the skin looks like. That is because shingles affects nerves, not just the outer layer of skin.
Typical shingles symptoms may include:
- Burning, tingling, or pain before the rash appears
- A one-sided stripe of rash or blisters
- Fluid-filled blisters that scab over in about a week
- Healing over two to four weeks
- Possible fever, headache, chills, or upset stomach
Shingles is not the kind of rash to casually ignore and hope it gets bored. Early treatment can shorten the illness, lower pain, and reduce the risk of long-lasting nerve pain called postherpetic neuralgia.
Why Shingles Is So Easy to Mistake for Something Else
Skin conditions love overlap. Many rashes itch. Many rashes hurt. Many rashes blister, crust, or turn red. That means a photo alone is often not enough to make a solid diagnosis. The body location, timing, pain pattern, exposure history, and whether the rash is one-sided or widespread all matter.
Some conditions mainly cause itch. Others mainly cause pain. Some spread because your skin touched a plant, soap, or allergen. Others follow a nerve path. Once you know what details to compare, the picture gets much clearer.
Conditions Commonly Mistaken for Shingles
1. Contact Dermatitis
Contact dermatitis happens when your skin reacts to something that touched it, such as a fragrance, metal, detergent, skin care product, or adhesive. It often causes redness, swelling, and itching. In some cases, it can also blister.
The main difference is that contact dermatitis usually itches more than it hurts. It also tends to show up exactly where the triggering substance touched the skin. If you changed laundry detergent, wore a new necklace, or used a new lotion and now the rash is parked in those areas, contact dermatitis becomes a strong possibility.
2. Poison Ivy, Poison Oak, or Poison Sumac
These rashes are basically the overachievers of itch. They can cause red, streaky, patchy skin with bumps and weeping blisters. The pattern often reflects where the plant brushed against the skin, so the rash may appear in lines or streaks rather than a neat one-sided band.
Poison ivy tends to be fiercely itchy, while shingles is more likely to be painful, burning, or tingling. If you spent the weekend gardening, hiking, or cleaning a yard and now have a streaky, very itchy rash, that history matters.
3. Herpes Simplex
Herpes simplex can also cause painful blisters that ooze and crust, which is why it sometimes gets mistaken for shingles. The difference is that herpes simplex usually causes smaller grouped blisters and tends to recur in the same general area, often around the mouth or genitals.
Shingles is more likely to create a broader band or patch that follows a nerve path on one side of the body. Herpes simplex is more about clustered sores than a stripe-like rash.
4. Cellulitis
Cellulitis is a bacterial skin infection. It can cause redness, warmth, swelling, and tenderness, sometimes with fever. People sometimes assume it is shingles because the area can be painful and alarming-looking.
But cellulitis usually looks more like a spreading red, hot, swollen area than a band of blisters. It does not typically start with tingling nerve pain and then turn into classic grouped vesicles. If the skin is rapidly expanding, hot to the touch, or you feel sick overall, cellulitis needs medical attention promptly.
5. Impetigo
Impetigo is a bacterial skin infection that often causes reddish sores that break open, ooze, and then form a honey-colored crust. It is especially common around the nose and mouth, though it can spread elsewhere.
If your rash looks crusty rather than nerve-like, and especially if it is around the face and seems more superficial than deeply painful, impetigo may be the better fit.
6. Eczema
Eczema is usually a story of dry, itchy, irritated skin that likes to come back when you least need the inconvenience. Some forms can blister or ooze, but eczema is usually more itchy, scaly, and recurrent than sharply painful.
It also tends to affect common areas such as the hands, inner elbows, behind the knees, or widespread patches, rather than forming a one-sided stripe that follows a nerve route.
7. Hives or Scabies
Hives can create raised, itchy welts that may move around or fade within hours. Scabies causes intense itch, often worse at night, with small bumps or lines in places like the wrists, waist, or finger webs. Neither one behaves like a classic shingles rash, but both can trigger the same “What in the world is happening to my skin?” reaction.
If the rash moves, shows up in multiple body areas, or itches far more than it hurts, shingles becomes less likely.
How Doctors Usually Tell the Difference
Doctors do not diagnose a rash by vibes alone. They look at the whole picture: where it started, how it feels, how fast it changed, whether it is one-sided, whether you had chickenpox in the past, and whether the rash fits a nerve distribution.
In many cases, shingles can be recognized from the rash pattern and symptoms alone. If the diagnosis is unclear, a clinician may test fluid from a blister to confirm the cause. That extra step can help separate shingles from herpes simplex or another blistering condition.
Doctors will also pay close attention to location. A rash near the eye, forehead, or nose can raise concern for eye involvement. If shingles affects the eye area, it can threaten vision and deserves urgent care.
Red Flags That Mean You Should Get Medical Care Quickly
Do not play wait-and-see with the following situations:
- The rash is on your face, especially near an eye
- You have eye redness, blurry vision, tearing, light sensitivity, or eye pain
- The rash is rapidly spreading or the skin is hot, swollen, and very tender
- You have fever or feel significantly ill
- You have a weakened immune system
- The pain is severe, even before many blisters appear
With shingles, antiviral treatment works best when started as soon as possible, ideally within the first few days after the rash appears. So if shingles is even on the short list of possibilities, getting checked early is smart, not dramatic.
If It Is Shingles, What Happens Next?
Treatment usually includes antiviral medication, pain management, and skin care. You may also be told to keep the rash clean and covered. Since direct contact with blister fluid can spread the virus that causes chickenpox to people who are not immune, covering the rash matters.
The rash itself often heals in a few weeks, but pain can linger. That lingering nerve pain is called postherpetic neuralgia, and it is one reason early treatment matters. In other words, shingles is not just a rash. It is a nerve problem wearing a rash costume.
How to Lower Your Risk of Shingles
The shingles vaccine, Shingrix, is recommended for adults age 50 and older and for certain immunocompromised adults age 19 and older. It is given as a two-dose series. It is one of the best tools available for preventing shingles and reducing the risk of complications.
If you have ever thought, “I’ll deal with that later,” this is your gentle nudge to move it up the list. Future You may send a thank-you note. Or at least fewer pain signals.
Bottom Line: Is It Shingles or Something Else?
If your rash is one-sided, painful, burning, tingling, and blistering, shingles should be taken seriously. If it is very itchy, widespread, streaky, hot and swollen, or recurring in the same tiny cluster, another condition may be more likely. The details matter, and timing matters even more.
When in doubt, especially with face or eye symptoms, get medical advice sooner rather than later. Skin can be confusing, but the right clues usually tell the story. The trick is knowing which clues to trust.
Real-World Experiences: When People Wonder, “Is It Shingles or Something Else?”
One common experience starts with pain before there is much to see. Someone notices a strange burning patch on one side of the ribs and assumes it is a pulled muscle, a bad bra band, or skin irritation from a shirt seam. A day or two later, small blisters appear in a narrow strip. That sequence, pain first and rash second, often surprises people because they expect a rash to look dramatic from the start. Instead, shingles may begin like a nerve complaint with a skin plot twist. By the time the blisters crust over, many people say the pain, not the appearance, was the part they underestimated.
Another very real scenario goes the other direction: the rash looks scary, but it turns out not to be shingles at all. A person spends an afternoon trimming bushes, pulling weeds, or cleaning up a backyard after a storm. Two days later, both forearms are covered in intensely itchy, streaky blisters. The first thought is often, “This has to be shingles.” But the giveaway is the itch and the plant exposure. Poison ivy and related rashes can look dramatic, leak fluid, and make life miserable, yet they usually do not come with that deep, one-sided nerve pain shingles is known for. They also love to show up in lines where the plant brushed the skin, which is a clue worth noticing.
Then there is the person who feels warmth, tenderness, and redness on a leg or arm and wonders whether shingles is the culprit because the area hurts. In some cases, the real issue is cellulitis, a skin infection that can spread quickly and make the skin look red, swollen, and hot. Instead of neat clusters of blisters, the skin may look more inflamed than blistered. People often describe it as “angry” skin that keeps expanding. That kind of experience is a reminder that not every painful rash is viral, and not every rash that looks alarming should be watched at home.
There are also people who deal with repeated blisters in the same area and assume shingles keeps coming back. Often, that pattern points more toward herpes simplex than shingles. The sores may start with tingling, break into small painful blisters, crust, and heal. Because the two conditions can share blistering and burning, the confusion is understandable. But shingles usually follows a broader nerve pathway and is less likely to behave like a frequent encore in the exact same tiny location.
What these experiences have in common is uncertainty. Most people are not trying to diagnose a textbook picture. They are trying to decode a real rash on a real Tuesday while also answering emails and wondering whether they need urgent care. That is why the practical clues matter so much: one-sided versus widespread, pain versus itch, nerve-like burning versus surface irritation, stripe versus streaks, and eye involvement versus no eye involvement. Those details often turn confusion into a clearer next step.





