Table of Contents >> Show >> Hide
- What Is Proton Beam Therapy, Exactly?
- Why Liver Cancer Is So Tricky to Treat
- Who May Benefit from Proton Beam Therapy for Liver Cancer?
- What the Evidence Says Right Now
- How Proton Beam Therapy Is Planned and Delivered
- Potential Benefits of Proton Beam Therapy
- Possible Downsides and Limitations
- Questions Patients Should Ask Their Care Team
- What the Experience Often Feels Like for Patients and Families
- Final Thoughts
Liver cancer treatment is rarely simple. If only tumors came with a user manual and the courtesy to stay still while you breathed. Instead, doctors often have to balance two goals at once: attack the cancer aggressively while protecting the liver tissue a patient still needs to live well. That balancing act is exactly why proton beam therapy has become such an important topic in modern liver cancer care.
Proton beam therapy is a specialized form of radiation that can deliver a highly focused dose to a tumor while reducing radiation exposure beyond the target. For liver tumors, that detail matters a lot. The liver sits near other organs that do not appreciate being caught in the crossfire, including the stomach, bowel, kidneys, bile ducts, and diaphragm. Many people with liver cancer also have cirrhosis or reduced liver function, which means there is less room for error and even less patience for collateral damage.
So, is proton beam therapy the magic answer? Not exactly. It is not a cure-all, not the right fit for every patient, and not always more appropriate than surgery, ablation, embolization, transplant, immunotherapy, or conventional photon-based radiation. But for carefully selected patients, proton beam therapy can be a smart, precise, and increasingly well-supported option. Think of it less like a silver bullet and more like a very expensive, very well-trained sniper.
What Is Proton Beam Therapy, Exactly?
Proton beam therapy is a type of external beam radiation therapy. Instead of using standard X-rays, also called photons, it uses positively charged particles called protons. The big selling point is physics. Protons can be planned to release most of their energy directly in the tumor and then stop, rather than continuing through the body with an “exit dose.”
For liver cancer, that feature is a big deal. Traditional radiation has become much better over the years, especially with techniques like IMRT and SBRT, but proton therapy may spare more healthy liver tissue in certain cases. That matters when the tumor is large, awkwardly located, close to critical structures, or sitting inside a liver that is already overworked by cirrhosis, hepatitis-related injury, or other chronic disease.
In plain English: proton therapy is designed to hit the cancer hard while being less rude to the healthy organs nearby.
Why Liver Cancer Is So Tricky to Treat
Most primary liver cancers are hepatocellular carcinoma, or HCC. Some patients also need radiation for intrahepatic cholangiocarcinoma or select liver metastases, but HCC is the main diagnosis in this conversation. What makes liver cancer difficult is that doctors are often treating two problems at once: the tumor itself and the condition of the underlying liver.
A patient may have a tumor that looks technically treatable, but poor liver reserve can make aggressive therapy risky. That is why treatment planning for liver cancer usually involves a multidisciplinary team, including hepatologists, surgeons, interventional radiologists, medical oncologists, transplant specialists, and radiation oncologists. Nobody gets extra points for pretending this is a one-doctor sport.
Small tumors may be managed with surgery, transplant, or thermal ablation. Intermediate or advanced cases may call for transarterial chemoembolization, radioembolization, systemic therapy, radiation, or combinations of those approaches. Proton therapy enters the picture when doctors believe radiation can help control the tumor while still respecting the limits of the surrounding liver and nearby organs.
Who May Benefit from Proton Beam Therapy for Liver Cancer?
Patients Who Are Not Good Candidates for Surgery
Some liver tumors cannot be removed safely because of size, location, vascular involvement, or the patient’s overall health. Others occur in people whose liver function makes surgery too risky. In those cases, radiation may be used as a definitive local treatment or as part of a broader treatment strategy.
Patients With Tumors Near Sensitive Structures
Proton therapy may be especially useful when a tumor is close to the stomach, bowel, porta hepatis, or other critical anatomy. It can also be attractive for irregularly shaped lesions or tumors located where normal tissue sparing is particularly important.
Patients With Limited Healthy Liver Reserve
For patients with cirrhosis or marginal liver function, reducing the dose to normal liver tissue is not just a technical victory; it can be the difference between a tolerable treatment and a dangerous one. This is one reason proton therapy continues to draw attention in HCC management.
Patients Being Considered for Bridging or Downstaging
In selected cases, radiation may be used to control a tumor while a patient awaits transplant, or to shrink or stabilize disease enough to make transplant or another curative option more realistic. Proton therapy is not the only way to do that, but it is increasingly discussed in that setting because of its ability to limit radiation to uninvolved liver tissue.
What the Evidence Says Right Now
The evidence for proton beam therapy in liver cancer is promising, but it is still evolving. That is the honest answer, and in cancer care honest answers are far more useful than shiny ones.
Prospective and multi-institutional studies have reported strong local control rates with proton therapy for unresectable liver tumors. In one widely cited phase II study of localized, unresectable HCC and intrahepatic cholangiocarcinoma, two-year local control for HCC was very high, with encouraging survival outcomes as well. Other studies have suggested that proton therapy can be used safely for large tumors and for challenging cases where preserving liver function is a major concern.
Reviews published in recent years have also pointed to a pattern: proton therapy appears particularly attractive when liver toxicity is the main worry. Some comparative data suggest a potential advantage over photon radiation in terms of liver-related toxicity and possibly survival in selected patients. But this is where nuance matters. The strongest possible proof still depends on randomized trials, and that level of evidence is not fully mature yet.
A phase III trial comparing proton therapy with photon therapy for liver cancer has been ongoing, and that is important because it aims to answer the question patients ask most: is proton actually better, or just fancier? Until final results are available, the safest conclusion is that proton therapy is a valuable option with strong rationale and encouraging outcomes, especially for selected patients, but it should not be marketed as automatically superior for every liver cancer case.
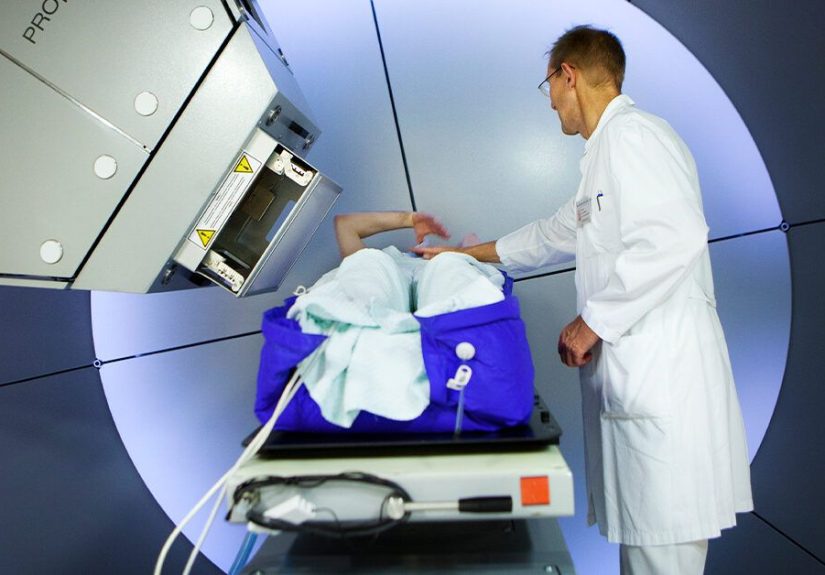
How Proton Beam Therapy Is Planned and Delivered
Proton therapy is not a one-size-fits-all process. Before treatment begins, patients usually have a consultation, imaging review, and planning session often called simulation. During simulation, the team creates a setup that can be reproduced with very high accuracy every day. That may include cushions, molds, breathing guidance, and imaging to account for tumor motion.
And yes, liver tumors move when you breathe. Very inconsiderate of them.
Because abdominal tumors shift with respiration, many centers use motion-management tools such as respiratory gating, breath-hold techniques, or four-dimensional imaging. The goal is to make sure the beam hits the intended target and not the neighborhood next door.
Treatment itself is usually outpatient. Patients often come in five days a week for several sessions, though the exact schedule varies by tumor type, dose, liver function, and institutional approach. The beam delivery is painless. Most of the session is spent on positioning and verification, while the actual radiation delivery may take only a few minutes.
Follow-up includes lab work, imaging, and clinical visits to assess tumor response and liver function over time. Proton therapy does not work like a light switch. Tumor response may unfold over weeks to months, and the care team monitors both effectiveness and toxicity carefully.
Potential Benefits of Proton Beam Therapy
- Better sparing of normal liver tissue in selected cases
- Reduced exit dose compared with photon radiation
- Useful for tumors near critical structures
- Can be an option for medically inoperable or unresectable disease
- May support bridging or downstaging strategies in select patients
- Noninvasive and usually performed as an outpatient treatment
Possible Downsides and Limitations
Proton therapy is impressive, but it is not magically free of tradeoffs.
First, availability is limited. Not every cancer center has proton equipment, and not every patient can travel easily to a specialized center. Second, insurance coverage can be complicated. Prior authorization is often required, and approval may depend on the diagnosis, the center, and whether the insurer agrees that proton therapy offers a meaningful benefit over photon radiation.
Third, side effects still exist. Patients may experience fatigue, skin irritation in the beam entry area, appetite changes, nausea, or other treatment-related effects depending on the portion of the liver and nearby organs being treated. Even when proton therapy reduces dose to healthy tissue, it is still radiation, not fairy dust.
Finally, not every tumor needs proton therapy. Some patients may do very well with standard photon SBRT, ablation, embolization, surgery, or systemic therapy. The best treatment is the one that fits the biology of the cancer, the condition of the liver, and the goals of care, not the one with the coolest brochure.
Questions Patients Should Ask Their Care Team
Is Proton Therapy Being Recommended Instead of, or Alongside, Another Treatment?
That question helps clarify whether proton therapy is intended to cure, control, bridge, downstage, or relieve symptoms.
Why Proton Instead of Photon Radiation?
The answer should be based on anatomy, liver reserve, expected toxicity, and the center’s expertise, not hype.
What Side Effects Are Most Likely in My Specific Case?
Side effects depend heavily on tumor location, liver function, prior treatments, and whether other therapies are being combined with radiation.
How Will You Manage Tumor Motion From Breathing?
This is especially relevant for liver tumors and says a lot about how carefully the plan is being tailored.
What Happens If Insurance Does Not Approve It?
Patients should know whether appeals are possible and what alternatives exist if proton therapy is not covered.
What the Experience Often Feels Like for Patients and Families
The experience of proton beam therapy for liver cancer is often a strange mix of high technology and very ordinary human emotions. On one hand, you are discussing pencil-beam scanning, motion management, dose constraints, and liver reserve. On the other hand, you are still a person trying to figure out whether you can eat dinner afterward, whether the parking garage is a maze designed by a villain, and whether the word “unresectable” is about to ruin your week.
For many patients, the first emotional hurdle is not the treatment itself but the decision-making process. They may hear about surgery from one specialist, ablation from another, embolization from a third, and proton therapy from a radiation oncologist who speaks fluent anatomy and mild optimism. That can feel overwhelming. Families often describe relief when a multidisciplinary team reaches a unified recommendation, because uncertainty is exhausting in a way no brochure fully captures.
Once treatment is chosen, the process tends to become more structured. Patients often say the planning appointment is the moment everything starts to feel real. There is imaging, positioning, marking, and a lot of “hold still, breathe normally, now hold your breath.” It can be oddly reassuring. The treatment plan begins to look less like an abstract cancer concept and more like a practical series of steps.
During the daily treatment phase, many people are surprised by how uneventful the sessions feel. There is no sensation when the proton beam is delivered. No zapping, no dramatic movie effects, no villainous sparks. Most of the effort goes into being lined up exactly the same way every day. That routine can become comforting. Patients often say that once they learn the flow of the center, know the faces of the staff, and understand the sounds of the machine, anxiety drops and the whole thing starts to feel manageable.
Fatigue can build gradually, and that sometimes catches people off guard. Not everyone feels wiped out, but some do notice that their energy becomes less reliable as treatment continues. Appetite may wobble. Some patients feel fine during treatment and then suddenly discover that the couch has become their most loyal companion by late afternoon. Families often end up adjusting schedules, meals, transportation, and work routines around that reality.
Another common part of the experience is the waiting. Waiting for insurance approval. Waiting for the start date. Waiting for follow-up scans. Waiting to hear whether the tumor shrank, stabilized, or merely decided to be mysterious. For caregivers, this period can be just as taxing as the treatment days themselves.
Still, many patients value proton therapy because it feels precise and purposeful. Even when the overall cancer journey is stressful, there is reassurance in knowing the team is trying to treat the tumor while protecting as much healthy liver as possible. That matters emotionally as much as medically. Patients are not only asking, “Will this work?” They are also asking, “What kind of life will I have while it works?” Proton therapy appeals to people because it speaks to both questions.
Final Thoughts
Proton beam therapy for liver cancer is one of the more compelling advances in modern radiation oncology. Its greatest strength is not that it replaces every other treatment, but that it gives clinicians another way to treat difficult tumors while better protecting normal tissue in the right clinical settings.
For patients with hepatocellular carcinoma or certain other liver tumors, especially those who are not surgical candidates or who have limited liver reserve, proton therapy may offer a meaningful local treatment option. The science behind it is strong, the clinical results so far are encouraging, and the real-world appeal is obvious. At the same time, the best approach remains individualized. Proton therapy is not the answer to every liver cancer case, but for the right patient, it may be a very smart answer to a very hard problem.