Table of Contents >> Show >> Hide
- What is thrombophlebitis?
- Symptoms: what thrombophlebitis feels (and looks) like
- Causes and risk factors: why clots and vein inflammation happen
- How thrombophlebitis is diagnosed
- Treatment: what actually helps (and what’s just wishful thinking)
- Prevention: keeping your veins calm and your blood moving
- Complications: what can happen if it’s ignored
- FAQ (because your brain will ask anyway)
- Experiences: what people commonly notice (and what tends to help)
If your body were a city, your veins would be the highway systemquietly moving traffic (blood) all day, every day. Thrombophlebitis is what happens when a blood clot (thrombo-) sets up camp inside a vein and the vein gets irritated and inflamed (-phlebitis). Think of it as a traffic jam and road rage, happening at the same time.
The tricky part: thrombophlebitis can be a minor, surface-level annoyance… or a sign of something more serious, like deep vein thrombosis (DVT), which can lead to a pulmonary embolism (PE). This guide breaks down thrombophlebitis symptoms, causes, and treatment options in plain American English, with just enough humor to keep your eyebrows relaxed.
What is thrombophlebitis?
Thrombophlebitis means a vein is inflamed because a clot is attached to the vein wall. It most commonly shows up in the legs, but it can appear in arms tooespecially around an IV line or catheter. Clinically, the big question is: Is the clot in a superficial vein (closer to the skin), or in a deep vein?
Superficial thrombophlebitis vs. deep vein thrombosis (DVT)
Superficial thrombophlebitis (also called superficial vein thrombosis) involves veins near the surface. It’s often painful and obvious, but usually less dangerous. DVT involves deeper veins and can be stealthiersometimes with subtle symptoms, sometimes with none at all. DVT matters more because the clot can break loose and travel to the lungs (PE).
Symptoms: what thrombophlebitis feels (and looks) like
Symptoms depend on whether the clot is superficial or deep. Your body is not subtle when a superficial vein is irritatedit’s basically waving a red flag. Deep veins, however, may whisper. (Rude.)
Symptoms of superficial thrombophlebitis
- Warmth and tenderness along a vein
- Redness and mild-to-moderate swelling in the area
- A firm, cord-like vein you can sometimes see or feel under the skin
- Pain that’s worse with pressure or when standing for long periods
Symptoms of deep vein thrombosis (DVT)
- Swelling (often in one leg or one arm)
- Pain or cramping, often in the calf or thigh
- Tenderness and warmth
- Skin may look redder or darker than usual
- Sometimes: no symptoms
When to treat it like an emergency
Seek emergency care immediately if you have symptoms that could suggest a pulmonary embolism, such as: sudden shortness of breath, chest pain (especially with breathing), coughing up blood, feeling faint, or a racing heartbeat. Don’t “wait and see” with breathing problemsthis is a “call now” situation.
Causes and risk factors: why clots and vein inflammation happen
Clots form when blood flow slows down, a vein is injured, or your blood becomes more likely to clot. In real life, these causes often team up like a trio of bad influences.
Common causes and triggers
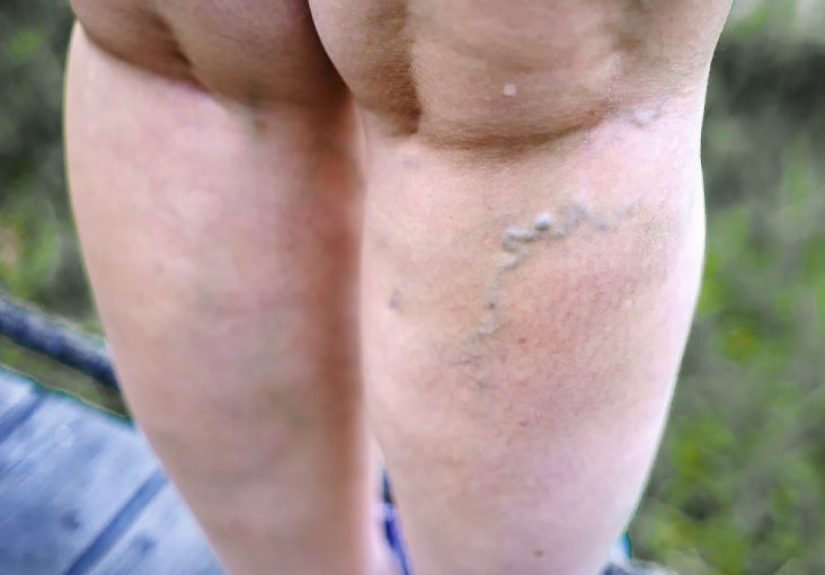
- Varicose veins (superficial veins that are stretched and twisty, where blood can pool)
- Injury to a vein, including trauma, surgery, or irritation from an IV line/catheter
- Long periods of immobility (bed rest, long travel, recovery after surgery)
- Hormonal factors (estrogen-containing birth control or hormone therapy)
- Pregnancy and the postpartum period
- Smoking (especially combined with estrogen-containing birth control)
- Cancer and some cancer treatments (including chemotherapy and central venous catheters)
- Clotting disorders (inherited or acquired)
- Chronic inflammatory or autoimmune conditions (for example, lupus)
- Obesity and increasing age (risk tends to rise over time)
A helpful way to think about risk is stacking: one risk factor might not cause trouble, but several at once can raise the odds. For example, a long flight plus dehydration plus estrogen therapy is like inviting a clot to a party and then acting surprised when it shows up.
How thrombophlebitis is diagnosed
A clinician will start with your symptoms and a physical exam, looking for warmth, redness, swelling, tenderness, and that classic “tender cord” of a superficial vein. But because DVT can masquerade as a muscle strainor hide completelytesting matters when the risk is higher.
Common tests
- Duplex ultrasound: the go-to test to look at blood flow and find clots, especially for suspected DVT
- Blood tests: sometimes used to evaluate clot risk or rule out other issues (your clinician decides what’s appropriate)
- Additional imaging: in select cases, especially if symptoms suggest complications or unusual clot locations
Treatment: what actually helps (and what’s just wishful thinking)
Treatment depends on the type and location of the clot, your symptoms, and your risk of complications. Some cases are handled with simple comfort measures, while others require prescription blood thinners. The goal is always the same: reduce pain and inflammation, prevent extension of the clot, and avoid dangerous complications.
Treatment for superficial thrombophlebitis
Many cases improve with conservative care. Typical recommendations may include:
- Warm compresses on the tender area
- Elevating the affected limb when resting
- NSAIDs (like ibuprofen or naproxen) if safe for you, to reduce pain and inflammation
- Compression stockings (especially for leg involvement) to support circulation
- Staying active (gentle walking helps blood flow; total stillness usually doesn’t)
If thrombophlebitis happens near an IV catheter, removing or changing the IV site is often part of management. In some higher-risk superficial clotssuch as clots that are extensive or close to where superficial veins connect to deep veinsclinicians may consider anticoagulation (blood thinners) to lower the risk of progression.
Treatment for deep vein thrombosis (DVT)
DVT is typically treated with anticoagulant medication to prevent the clot from growing and reduce the risk of PE. Depending on the situation, therapy might involve different classes of blood thinners and a specific duration (often measured in months, not days). Your care team weighs clot risk against bleeding riskbecause blood thinners can be life-saving, but they’re not casual.
In selected casesespecially large clots, severe symptoms, or certain high-risk scenariosspecialized procedures may be considered, such as catheter-based treatments to remove or break up a clot. These are not “standard for everyone,” but they exist for specific clinical reasons.
Home care tips that are actually useful
- Move regularly: short walks beat marathon couch sessions. If pain limits movement, ask your clinician what’s safe.
- Use compression correctly: “correctly” means proper size and fitcompression that’s too tight can cause problems.
- Know your medication rules: if you’re prescribed anticoagulants, follow dosing exactly and ask about drug interactions.
- Don’t massage the area: it’s tempting, but pressure over a clot isn’t a great DIY experiment.
Prevention: keeping your veins calm and your blood moving
You can’t control every risk factor (aging is surprisingly non-negotiable), but you can reduce the odds of thrombophlebitis and DVT. Prevention focuses on minimizing immobility, improving circulation, and managing known risks.
Practical prevention strategies
- During long travel: if you’re traveling for more than a few hours, move your legs often and walk when you can. Flex and extend your ankles, and avoid staying pinned in one position.
- After surgery or hospitalization: follow mobility and prevention instructions (walking, compression devices, prescribed meds).
- Manage modifiable risks: smoking cessation, staying hydrated, and addressing weight and activity levels when possible.
- Talk about hormones: if you use estrogen-containing birth control or hormone therapy and have clot risk factors, ask your clinician about safer options.
- Know your family history: recurrent clots or early clots in relatives may point to inherited risk.
Complications: what can happen if it’s ignored
Superficial thrombophlebitis is often self-limited, but it’s not always harmlessespecially if it’s extensive or near deep-vein connections. DVT can lead to pulmonary embolism, and can also cause longer-term issues like post-thrombotic syndrome (chronic swelling, discomfort, skin changes) when vein valves are damaged.
FAQ (because your brain will ask anyway)
Is thrombophlebitis the same as a blood clot?
Thrombophlebitis involves a clot plus inflammation of the vein. Not every clot causes noticeable inflammation, and not every sore vein means there’s a clothence the importance of evaluation when risk is higher.
Can I treat superficial thrombophlebitis at home?
Sometimes, yesespecially when symptoms are mild and you have low risk factors. Warm compresses, elevation, and NSAIDs may help. But if symptoms are worsening, spreading, or you have DVT risk factors, get medical advice. “It’s probably fine” is not a diagnostic test.
How long does it take to get better?
Superficial symptoms may improve over days to a couple of weeks, though some tenderness can linger. DVT treatment is typically longer and depends on your individual situation and risk factors.
Experiences: what people commonly notice (and what tends to help)
Let’s talk about the human sidebecause thrombophlebitis isn’t just a definition in a textbook; it’s a very real “Why is my leg doing this?” moment. While everyone’s story is different, there are patterns clinicians hear again and again.
Experience #1: The “I thought it was a pulled muscle” phase. People with early DVT symptoms often describe a deep ache or cramp that feels like they overdid leg dayexcept they didn’t. It might show up after a long drive, a flight, or a few days of being less mobile than usual (illness, work crunch, recovery after surgery). A common detail: the discomfort doesn’t behave like typical soreness. Stretching doesn’t fix it. Rest doesn’t fully fix it. And it may gradually become more noticeable, especially with swelling in one limb.
Experience #2: The “angry red line” that practically introduces itself. Superficial thrombophlebitis can be more obvious: a tender, warm, red area along a veinsometimes with a firm “cord” underneath the skin. People often say it’s sore to the touch and annoying when standing, but they feel otherwise okay. Some notice it after an IV placement (the arm near the catheter site becomes tender and inflamed), or after a period of inactivity. It can look dramatic even when the overall risk is low, which is why a proper check matters: appearances can be misleading in both directions.
Experience #3: The relief of “simple” measureswhen appropriate. For superficial cases, people often report that warm compresses feel surprisingly effective. The heat can soothe local irritation, and elevation can reduce that heavy, throbbing sensation. Many also find that gentle walkingshort, frequent movement rather than heroic workoutshelps the limb feel less stiff. Compression stockings can be a love/hate relationship: when fitted correctly, they often reduce swelling and discomfort; when fitted poorly, they can feel like a medieval punishment device. If you try compression, sizing matters.
Experience #4: The “medication learning curve.” Anyone placed on anticoagulants (for DVT or higher-risk superficial clots) often describes a mental adjustment: being careful with missed doses, understanding bleeding signs, and checking interactions with other medications. It’s not scary once you’re informed, but it does require attention. Many people feel better emotionally once they understand the purpose: anticoagulants don’t always “dissolve” the clot overnight; they prevent growth and lower the risk of dangerous travel. Your body can gradually break down the clot over time.
Experience #5: The power of “I came in early.” People who seek care quicklyespecially when swelling is one-sided, pain escalates, or risk factors are presentoften avoid complications and get clarity faster. Ultrasound can turn anxiety into a plan: either reassurance and conservative care, or treatment that prevents the situation from getting worse. The most consistent takeaway from real-world stories is simple: if something feels off and the risk is there, getting checked is a win, even if the result is “good news.”
A friendly reminder: experiences are helpful for recognition, but they’re not a substitute for diagnosis. If you suspect thrombophlebitis or DVTespecially with chest symptoms or shortness of breathget medical care promptly.