Table of Contents >> Show >> Hide
- What Is a Nebulizer?
- How Does a Nebulizer Work?
- Types of Nebulizers
- Who Uses a Nebulizer?
- What Medicines Can Be Used in a Nebulizer?
- Nebulizer vs. Inhaler: Which Is Better?
- How to Use a Nebulizer Correctly
- How to Clean a Nebulizer
- Common Mistakes to Avoid
- When to Talk to a Healthcare Professional
- Real-World Experiences With Nebulizers
- Final Thoughts
If you have ever heard someone say, “Grab the breathing machine,” they were probably talking about a nebulizer. It is not the flashiest device in the respiratory world. It does not fit in your jeans pocket like a tiny inhaler. It does not win points for glamour. But when someone needs medicine delivered straight to the lungs in a gentle, steady mist, a nebulizer can be a very useful tool.
Whether you are managing asthma, living with COPD, caring for a child with wheezing, or just trying to decode the mountain of instructions that came with your machine, understanding how a nebulizer works can make treatment less stressful. And yes, less “What on earth is this tubing for?”
In this guide, you will learn what a nebulizer is, the main types of nebulizers, who uses them, what medicines may be delivered through them, how to clean one correctly, and what everyday use often feels like in real life.
What Is a Nebulizer?
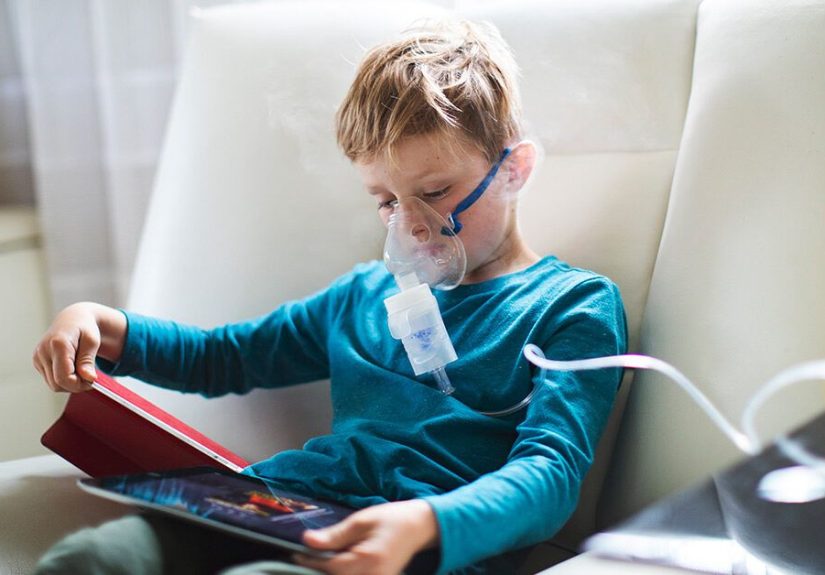
A nebulizer is a device that turns liquid medication into a fine mist so you can breathe it deep into your lungs. Instead of timing a puff from an inhaler with your inhale, you usually sit upright, place a mouthpiece in your mouth or a mask over your nose and mouth, and breathe normally while the machine does the work.
That simple difference matters. A nebulizer is not medicine by itself. It is a delivery system. Think of it as the taxi, not the passenger. The medication is the active treatment, and the nebulizer helps carry that treatment into the airways.
Nebulizers are often used for people with asthma, chronic obstructive pulmonary disease (COPD), cystic fibrosis, bronchiectasis, and other chronic lung conditions. They may also be prescribed when someone is having trouble using an inhaler correctly, needs a specific nebulized medication, or benefits from a slower, mist-based treatment.
How Does a Nebulizer Work?
A typical nebulizer has a few basic parts: the machine or power unit, tubing, a medicine cup, and either a mouthpiece or face mask. You pour the prescribed liquid medication into the medicine cup, connect the parts, turn on the device, and inhale the mist until the cup is empty.
Most treatments take around 5 to 15 minutes, though some may run a little longer depending on the device, the medication volume, and the type of nebulizer you are using. The process is usually calm and straightforward: sit upright, keep the cup in the correct position, and breathe in the mist steadily until it stops.
One important point: a nebulizer only works well when it is used the right way. Loose mask fit, poor positioning, skipped cleaning, or mixing medicines without professional instructions can all reduce how well the treatment works.
Types of Nebulizers
Not all nebulizers are built the same. The three main types are jet nebulizers, ultrasonic nebulizers, and mesh nebulizers.
1. Jet Nebulizers
Jet nebulizers are the classic workhorses. They use compressed air to turn liquid medicine into a mist. These are common in homes, clinics, and hospitals. They are reliable, widely available, and often less expensive than newer designs. The trade-off is that they can be a little bulky and noisy. If yours sounds like a tiny leaf blower with a medical degree, that is pretty normal.
2. Ultrasonic Nebulizers
Ultrasonic nebulizers use high-frequency sound vibrations to create the mist. They are usually quieter than jet models, which can be a huge bonus for children, light sleepers, and anyone who already feels grumpy before a morning treatment. Some medications and formulations may work better in certain devices than others, so it is important to follow the manufacturer’s guidance and your clinician’s instructions.
3. Mesh Nebulizers
Mesh nebulizers push medication through a very small mesh to make a fine mist. These devices are often compact, portable, and easier to travel with. Many people like them because they are quieter and more convenient. They also tend to cost more, and some need more careful cleaning to keep the mesh from clogging.
Who Uses a Nebulizer?
Nebulizers are prescribed for both children and adults. They are especially useful for infants, young children, older adults, or people who are very ill and cannot coordinate inhaler use well. If taking a deep, timed puff from an inhaler feels like trying to clap and juggle at the same time, a nebulizer can be the easier option.
Common situations where a nebulizer may be used include:
- Asthma: Especially for young children, severe symptoms, or people who struggle with inhaler technique.
- COPD: Some bronchodilator medicines for COPD are available in nebulized form.
- Cystic fibrosis: Nebulized medications may help manage thick mucus and infections as part of a broader care plan.
- Bronchiectasis: Some patients use nebulized saline or mucolytic therapies to help loosen secretions.
- Short-term respiratory flare-ups: In some cases, providers may prescribe nebulized treatments during periods of worsening symptoms.
That said, a nebulizer is not automatically “better” than an inhaler. For many people, inhalers work extremely well when used correctly. The best device depends on the person, the medication, the diagnosis, and how likely the medicine is to actually reach the lungs the way it should.
What Medicines Can Be Used in a Nebulizer?
The exact medication depends on your prescription, but nebulizers commonly deliver a few broad categories of treatment.
Bronchodilators
These medicines help open the airways. Albuterol and levalbuterol are common examples. Some patients with COPD may use ipratropium or a combination such as albuterol and ipratropium. These are often used to relieve wheezing, chest tightness, or shortness of breath.
Inhaled Corticosteroids
Some nebulized medicines reduce airway inflammation rather than giving rapid symptom relief. Budesonide is a well-known example. This type of medicine is used more as a controller treatment than as a rescue medicine. If a nebulized corticosteroid is used, patients are usually advised to rinse the mouth afterward, and children using a mask may also need their face washed.
Saline and Mucus-Thinning Treatments
Depending on the condition, a provider may prescribe sterile saline or mucolytic medication to help loosen thick mucus. This is more common in conditions such as cystic fibrosis or bronchiectasis, where airway clearance is a major part of daily care.
Important Safety Note
Do not pour random liquids into a nebulizer. No homemade blends. No mystery drops from the back of the cabinet. No “my cousin saw this online” experiments. Only use medication or solution specifically prescribed or recommended for nebulizer use. Also, do not mix nebulized medications unless your doctor or pharmacist tells you it is safe to do so.
Nebulizer vs. Inhaler: Which Is Better?
The honest answer is: neither is universally better. They are just different tools.
A nebulizer may be better when:
- The patient is too young or too sick to use an inhaler properly.
- A face mask is easier than coordinating inhaler technique.
- A specific medicine is prescribed in nebulized form.
- The person needs a slower treatment with normal breathing rather than timed inhalation.
An inhaler may be better when:
- Portability and speed matter.
- The patient has good technique.
- The medication is available in inhaler form.
- Quick, on-the-go treatment is needed.
In many cases, the choice comes down to what the patient can use correctly and consistently. A perfectly prescribed medicine does not help much if it never makes it into the lungs.
How to Use a Nebulizer Correctly
General steps usually look like this:
- Wash your hands.
- Assemble the machine, tubing, medicine cup, and mask or mouthpiece.
- Add the prescribed medication to the cup.
- Sit upright.
- Place the mouthpiece between your lips or fit the mask snugly over the nose and mouth.
- Turn on the machine.
- Breathe calmly and steadily through your mouth until the mist stops.
- If the medicine is an inhaled corticosteroid, rinse your mouth and spit out the water. If a mask was used, wash the face too.
Always read the instructions for your specific device because setup and cleaning can vary by model. A jet nebulizer, mesh nebulizer, and pediatric mask setup do not always play by the exact same rules.
How to Clean a Nebulizer
This is the part many people want to skip, but it is one of the most important parts of treatment. A poorly cleaned nebulizer can collect germs, and the last thing a person with lung disease needs is a dirty device blowing unwanted microbes straight toward the airways. Not ideal. Zero stars.
After Each Use
- Take the nebulizer apart.
- Wash the medicine cup and mouthpiece or mask with warm water and mild soap, if your manufacturer allows it.
- Rinse well.
- Let the parts air-dry on a clean surface or paper towel.
- Do not wash the tubing unless your manufacturer specifically says it is safe.
Weekly Disinfection
Many devices also need regular disinfection, often once a week or more often if your care team instructs it. Depending on the device and manufacturer instructions, approved methods may include:
- Soaking in a vinegar-and-water solution for a set time.
- Using 70% isopropyl alcohol or 3% hydrogen peroxide for certain reusable parts.
- Boiling, using a dishwasher hot cycle, microwaving in water, or using an electric steam sterilizer if the device materials allow it.
The catch is that not every method works for every machine. Some specialty care programs, including cystic fibrosis guidance, are especially strict about prompt cleaning, disinfection, rinsing, and thorough air-drying. For some cold-disinfection methods, sterile water may be recommended for rinsing afterward instead of tap water. So yes, this is one of those moments where the manufacturer’s booklet actually deserves your attention.
Storage Tips
- Store dry parts in a clean, dry container or bag.
- Keep the machine in a cool, dry place.
- Replace filters or accessories according to the device instructions.
- Check tubing, mask, and cups for wear, cracks, or discoloration.
Common Mistakes to Avoid
- Using leftover medicine from a previous treatment.
- Mixing medications without medical guidance.
- Skipping regular cleaning and disinfection.
- Using the wrong mask size or a loose-fitting mask.
- Lying down flat during treatment unless specifically instructed.
- Assuming every breathing problem needs a nebulizer.
- Thinking a controller medicine will act like a rescue treatment.
If your symptoms are getting worse, your medicine does not seem to help, or the machine suddenly sounds strange and produces little or no mist, it is time to contact your healthcare team or equipment provider.
When to Talk to a Healthcare Professional
Contact your clinician if you are using rescue medication more often than usual, waking up short of breath, having more wheezing, coughing more at night, or feeling that treatments are not working the way they used to. People with asthma or COPD often need their treatment plan reviewed when symptom patterns change.
Seek urgent medical care right away for severe trouble breathing, blue lips, confusion, inability to speak in full sentences, or symptoms that continue to worsen despite rescue treatment.
Real-World Experiences With Nebulizers
One reason nebulizers remain so common is that they fit real life, not just textbook life. In everyday use, people often describe the experience less as “medical technology” and more as “a routine I had to learn, then eventually stopped thinking about.” That shift matters.
For parents of young children with asthma, the first few treatments can feel like a negotiation with a tiny union representative who strongly opposes face masks. A toddler may cry, pull at the mask, or refuse to sit still. Over time, many families build rituals around treatment: one favorite book, one cartoon episode, one stuffed animal, one chair, same time every day. The nebulizer becomes less of a dramatic event and more of a predictable pause in the routine.
Adults with COPD often describe a different experience. For them, the nebulizer may feel like part of a larger morning system: wake up, sit upright, take treatment, cough out mucus, drink water, and get moving slowly. Some say the treatment itself is not difficult, but cleaning the device and keeping supplies organized is the real challenge. In other words, the medicine may be quick, but the maintenance has opinions.
People who switch from inhalers to nebulizers sometimes notice that treatments feel slower but easier. They do not have to coordinate a perfect inhale at the exact second a puff is released. That can be a huge relief for older adults, people with fatigue, and anyone having a rough breathing day. The downside is convenience. A portable inhaler can go almost anywhere. A tabletop nebulizer is more of a “we are staying here for 10 minutes” commitment.
Portable mesh nebulizers change that experience for some users. Travelers and busy caregivers often appreciate quieter devices that fit into a bag and do not sound like a small vacuum cleaner. But these devices also tend to require careful cleaning, especially around the mesh, and that can frustrate users who want something fast and foolproof.
Another common experience is that people do not realize how important cleaning is until a respiratory therapist, nurse, or pharmacist explains it clearly. Once patients understand that moisture plus medication residue plus poor drying can create a germ-friendly setup, cleaning stops feeling like a fussy extra and starts feeling like part of the treatment itself.
Perhaps the biggest real-world lesson is this: people do best when the nebulizer fits into a realistic routine. The best setup is not the one that looks perfect in an instruction manual. It is the one a family can keep doing correctly on a busy Tuesday, during allergy season, when the dog is barking, the phone is ringing, and somebody still has to make dinner.
Final Thoughts
A nebulizer is a practical, effective way to deliver certain medications straight into the lungs. It can be especially helpful for children, older adults, people with chronic lung disease, and anyone who struggles with inhaler technique. The right device, the right medication, and the right cleaning habits can make a big difference in how well treatment works.
The short version? A nebulizer is not magic, but it can be a very good teammate. Use only prescribed medication, follow your device instructions, clean it like you mean it, and check in with your healthcare team when symptoms or routines change.