Table of Contents >> Show >> Hide
- Hairy Cell Leukemia, Explained (Without the Jargon)
- Symptoms of Hairy Cell Leukemia
- What Causes Hairy Cell Leukemia?
- How Hairy Cell Leukemia Is Diagnosed
- Treatment Options for Hairy Cell Leukemia
- What Recovery and Follow-Up Can Look Like
- Living With Hairy Cell Leukemia: The Big Picture
- of Real-World Experiences (What Patients and Caregivers Often Describe)
- Conclusion
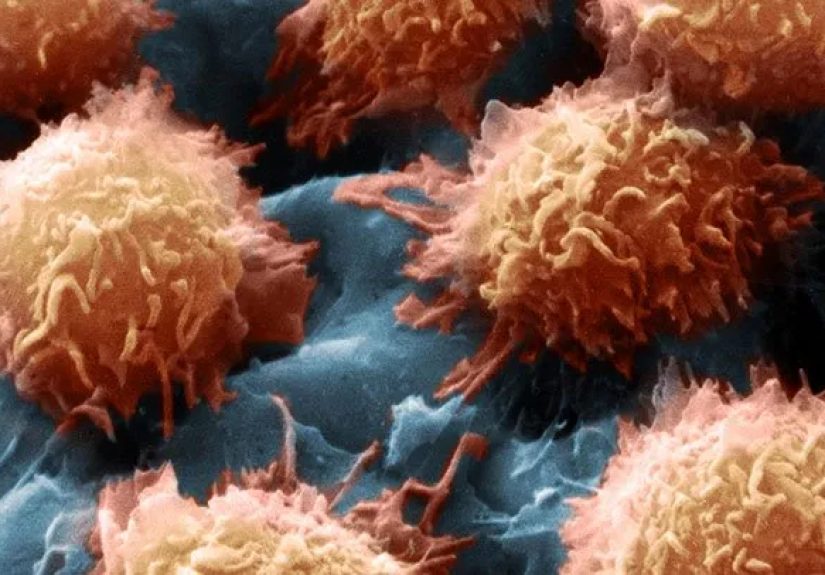
Hairy cell leukemia sounds like something a cartoon villain would invent. In real life, it’s much less dramatic-looking (and much more treatable) than the name suggests. Hairy cell leukemia (HCL) is a rare, slow-growing blood cancer that starts in certain white blood cells called B lymphocytes. Under a microscope, the abnormal cells can look like they have tiny “hairy” projectionshence the nickname. Those “hairs” aren’t a style choice; they’re part of what helps doctors recognize the disease.
The good news: for many people, HCL responds extremely well to treatment and can stay under control for years at a time. Many patients go long stretches without needing additional therapy. The not-so-fun part: it can quietly lower blood counts and increase infection risk if it progresses untreated. Let’s break down what HCL is, what symptoms to watch for, why it happens, and what treatment typically looks like today.
Hairy Cell Leukemia, Explained (Without the Jargon)
Hairy cell leukemia is a chronic B-cell leukemia, meaning it usually develops slowly rather than racing through the body. Most hairy cells collect in the bone marrow (where blood cells are made) and the spleen (a blood-filtering organ). Over time, these abnormal cells crowd out healthy blood-forming cells, which can cause low levels of:
- Red blood cells (leading to anemia and fatigue)
- White blood cells (raising infection risk)
- Platelets (making bruising or bleeding more likely)
HCL is considered rare. It’s diagnosed more often in adults than in kids, and it tends to affect men more frequently than women. There are also related conditions that can look similar, including hairy cell leukemia variant (HCL-V), which behaves differently and may respond differently to certain treatments. That’s one reason accurate diagnosis matters so much.
Symptoms of Hairy Cell Leukemia
Hairy cell leukemia often starts quietly. Some people find out they have it after routine bloodwork, with no symptoms at all. When symptoms do happen, they usually come from low blood counts or an enlarged spleen.
Common symptoms
- Fatigue or low energy (often from anemia)
- Frequent infections or infections that hit harder than usual
- Easy bruising or bleeding (such as nosebleeds or bleeding gums)
- Shortness of breath with activity
- Feeling full quickly when eating (from an enlarged spleen pressing on the stomach)
- Abdominal fullness or discomfort, usually on the left side
- Unexplained weight loss or fevers (less common, but possible)
One classic clue doctors look for is a type of low white blood cell called monocytopenia (low monocytes) along with other low counts. But symptoms alone can’t confirm HCLmany conditions can cause fatigue or infectionsso testing is key.
What Causes Hairy Cell Leukemia?
Hairy cell leukemia happens when a B cell develops DNA changes (mutations) that tell it to grow and survive when it shouldn’t. For most people with “classic” hairy cell leukemia, a specific mutation called BRAF V600E is involved. This mutation affects a growth-signaling pathway inside the cell, basically pushing the cell’s “go” button too often.
Here’s the important nuance: having a mutation in the leukemia cells does not mean you inherited it or that you did anything wrong. These mutations are typically acquired during life in the cancer cellsnot passed down through families.
Risk factors (and what we actually know)
HCL is rare enough that risk factors aren’t as clear-cut as they are for some other conditions. Still, research and clinical observations suggest a few patterns:
- Age: It’s more common in middle-aged and older adults.
- Sex: It’s diagnosed more often in men.
- Certain exposures: Some sources note an association between HCL and Agent Orange exposure. Association doesn’t always prove cause, but it’s an important point to discuss with your healthcare team if it applies.
In many cases, doctors can’t point to one specific cause. The practical takeaway is that HCL is best understood as a combination of acquired genetic changes in B cells plus factors we don’t fully understand yet.
How Hairy Cell Leukemia Is Diagnosed
Diagnosis usually involves a mix of blood tests and bone marrow testing. Because HCL can overlap with other blood cancers, doctors rely on a “fingerprint” approach: what the cells look like, how they behave, and which markers they carry on their surface.
Tests you might hear about
- Complete blood count (CBC): Checks red cells, white cells, and platelets. HCL often shows low counts (pancytopenia).
- Peripheral blood smear: A lab professional examines blood cells under a microscope. Sometimes “hairy” cells are visible.
- Bone marrow biopsy: Helps confirm diagnosis and shows how much the marrow is affected.
- Flow cytometry: A highly useful test that identifies cell surface markers typical of HCL.
- Genetic/molecular testing: Often checks for BRAF V600E (especially in classic HCL), which can also guide treatment choices.
- Imaging (like CT): May be used to evaluate spleen size or other findings.
Because treatment decisions depend on whether this is classic HCL, HCL variant, or another similar disorder, getting evaluated by a hematologist (often one familiar with rare leukemias) can be a real advantage.
Treatment Options for Hairy Cell Leukemia
Hairy cell leukemia is one of those cancers where the treatment story is often encouraging: many patients respond very well, and remissions can last for years. Treatment isn’t always immediate, though. A lot depends on symptoms, blood counts, infections, and spleen size.
When doctors recommend treatment
Many clinicians treat HCL when there are signs the disease is causing problems, such as:
- Symptomatic anemia (fatigue, shortness of breath tied to low red cells)
- Low white blood cells with infections or high infection risk
- Low platelets with bleeding/bruising risk
- Growing spleen causing discomfort or early fullness
- Other complications related to progression
Watchful waiting (yes, sometimes “doing nothing” is a plan)
If you feel well and your blood counts are stable, your doctor may recommend active surveillance (often called watchful waiting). That means regular checkups and lab work, with treatment saved for when it’s truly needed. It’s not neglectit’s strategy. Many people prefer to delay therapy until the benefits clearly outweigh the downsides.
First-line therapy: purine analogs
For decades, the backbone of HCL treatment has been a class of medicines called purine analogs, most commonly:
- Cladribine
- Pentostatin
These treatments are highly effective for classic HCL. They can be given in different schedules depending on the drug and the clinical situation. One important reality: purine analogs can temporarily weaken the immune system, so doctors pay close attention to infection riskespecially if someone already has an active infection at the time treatment is needed.
Adding immunotherapy: rituximab (and sometimes other anti-CD20 antibodies)
Rituximab is an antibody therapy that targets a marker on B cells. It may be used in combination with cladribine (either sequentially or concurrently in some approaches), or used in certain relapse situations. The idea is to deepen remissionmeaning fewer residual leukemia cells left behindespecially for patients with higher-risk features or those who relapse.
Targeted therapy for BRAF-positive disease
Because classic HCL often involves BRAF V600E, targeted therapy has become a major toolparticularly for relapsed/refractory disease or when standard chemo-like options aren’t ideal.
Targeted approaches may include:
- BRAF inhibitors such as vemurafenib or dabrafenib
- MEK inhibitors (like trametinib) in certain combinations, depending on the situation
These treatments aim at the signaling pathway that helps leukemia cells survive. In some cases, doctors may pair a targeted drug with rituximab to strengthen the response.
Other options in relapsed or special situations
Depending on your history, your test results, and what’s available, additional options may include:
- Ibrutinib (a BTK inhibitor) in select cases
- Interferon-alpha (sometimes considered when other options aren’t suitable, including certain infection scenarios)
- Splenectomy (removal of the spleen), which is much less common today but still occasionally considered
- Clinical trials exploring chemo-free strategies and newer antibodies
Note on moxetumomab pasudotox (Lumoxiti): This anti-CD22 therapy was FDA-approved for relapsed/refractory HCL in the past, but it was later permanently withdrawn from the U.S. market for commercial reasons. If you see it mentioned online, ask your doctor about current availability and modern alternatives.
What Recovery and Follow-Up Can Look Like
Hairy cell leukemia treatment is often a “one-and-done for a while” experienceespecially after first-line therapy. But follow-up matters because HCL can come back over time.
After treatment: what doctors monitor
- Blood counts over time (CBC trends)
- Symptoms (fatigue, infections, bruising)
- Spleen size and physical exam findings
- Sometimes bone marrow testing or specialized labs if relapse is suspected
Because immune recovery can take time after certain therapies, your care team may also talk with you about vaccines, infection prevention, and when to call in early for fevers or unusual symptoms.
Living With Hairy Cell Leukemia: The Big Picture
HCL is often described as “highly treatable,” and that lines up with what many patients experience: long remissions, strong responses to therapy, and a life that can look pretty normal between checkups. Still, it’s cancerand it can bring stress, uncertainty, and real day-to-day challenges like fatigue or infection anxiety.
If you take nothing else away, take this: you don’t have to guess. If your blood counts are off, you’re having frequent infections, or you’re dealing with unexplained fatigue plus easy bruising, it’s worth getting evaluated. Early clarity tends to beat late surprises.
of Real-World Experiences (What Patients and Caregivers Often Describe)
Because hairy cell leukemia can develop slowly, a common “experience story” starts with something ordinarylike a routine physical or lab work for an unrelated issue. People often describe being blindsided by the phrase “leukemia” because they didn’t feel dramatically sick. One patient might say they were just “tired all the time,” assuming it was stress, work, school, or not sleeping enough. Another might remember getting infections back-to-backsinus infection, then bronchitis, then another “mystery fever”and realizing their immune system wasn’t bouncing back like it used to.
Many patients describe the diagnosis process as both frustrating and reassuring. Frustrating because it can take multiple testsrepeat blood draws, referrals, then a bone marrow biopsyto get a confident answer. Reassuring because once the hematologist explains that hairy cell leukemia is often very responsive to treatment, the emotional tone can shift from panic to problem-solving. People often say the first big relief is simply having a name for what’s been happening.
Treatment experiences vary, but a lot of patients share a similar pattern: the therapy itself can feel manageable, while the “after” period requires patience. For example, someone might feel okay during cladribine or pentostatin but then notice their energy comes back in stages, not overnight. It’s common to hear: “I expected to feel normal in two weeks, and instead it took a couple months to really feel like myself.” That doesn’t mean the treatment failedit often means the body needs time to rebuild healthy blood counts and immune function.
Another recurring theme is learning to treat infection prevention like a skill, not a personality trait. Patients and families often talk about becoming more intentional: washing hands like it’s a sport, being cautious around sick friends, and calling the clinic sooner when a fever pops up instead of trying to “tough it out.” Some people also describe the mental balancing act of staying careful without letting cancer run the entire calendar.
Long remissions can bring their own emotional curve. When life returns to normal, some people feel guilty for not thinking about it; others feel uneasy because it’s quietlike waiting for the other shoe to drop. Many find it helpful to build a simple routine around follow-ups: keep a list of symptoms to mention, track CBC trends, and write down questions before appointments. That kind of structure can turn anxiety into a plan.
If you’re supporting someone with HCL, caregivers often say the most helpful thing is being steady and practical: driving to appointments, helping keep track of medications, and offering low-pressure support (“Want company on a short walk?”) rather than forced optimism. And for patients: it’s okay to need time. Recovery isn’t a straight line, but for many people with hairy cell leukemia, it’s a path that leads back to a full lifejust with a few more lab results in the story.
Conclusion
Hairy cell leukemia is a rare, slow-growing B-cell blood cancer that often responds extremely well to modern therapy. Symptoms commonly relate to low blood counts and an enlarged spleen, and many cases involve the BRAF V600E mutation that can guide targeted treatment. If you’re diagnosed, your care plan may include watchful waiting, purine analog therapy (cladribine or pentostatin), immunotherapy like rituximab, or targeted options in relapse. With the right monitoring and care, many people live well with HCL for years.