Table of Contents >> Show >> Hide
- What Is Alopecia Areata?
- How Alopecia Areata Fits Into the Bigger Hair Loss Picture
- What Causes Alopecia Areata?
- Common Signs and Symptoms
- How Doctors Diagnose Alopecia Areata
- Treatments for Alopecia Areata
- Tips to Cope With Alopecia Areata Day to Day
- What Living With Alopecia Areata Often Feels Like
- Final Thoughts
Hair loss has a special talent for showing up uninvited, usually right when your confidence was finally minding its own business. One day you are brushing your hair like a normal person, and the next day you are inspecting a suspicious patch in the mirror like a detective on a budget. If that patch turns out to be alopecia areata, the experience can feel confusing, emotional, and a little surreal.
The good news is that alopecia areata is better understood than it used to be, and treatment options have expanded in a big way. The not-so-fun news is that it is still unpredictable. This guide breaks down what alopecia areata is, what causes it, how doctors treat it, and what real coping can look like when your hair seems to be freelancing without permission.
What Is Alopecia Areata?
Alopecia areata is an autoimmune form of hair loss. In plain English, that means your immune system gets a little confused and starts targeting your hair follicles instead of behaving like the responsible adult in the room. The result is usually sudden, patchy hair loss that can appear on the scalp, beard area, eyebrows, eyelashes, or other parts of the body.
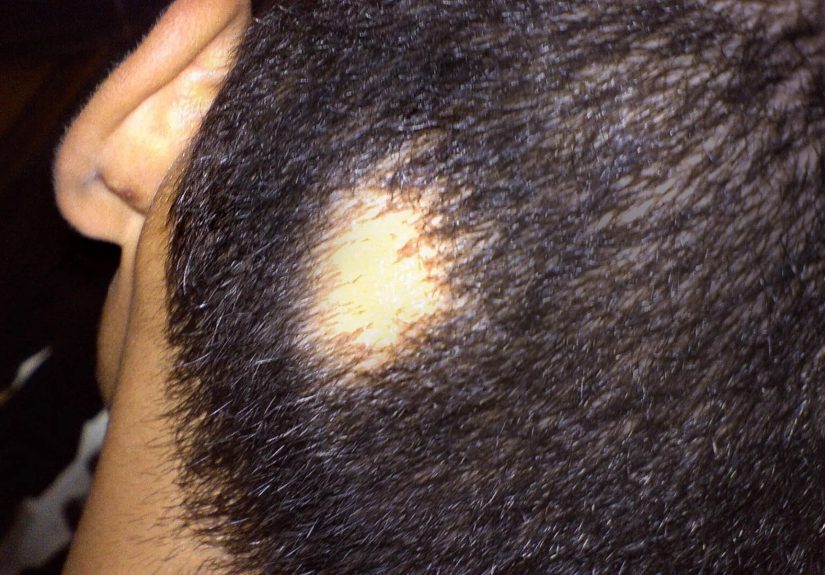
One of the key things that makes alopecia areata different from some other hair loss conditions is that the affected skin often looks smooth. There is usually no scarring, no obvious rash, and no dramatic irritation. Many people first notice small round or oval bald spots, though some people lose more extensive amounts of hair over time.
Alopecia areata can show up in a few forms:
- Patchy alopecia areata: the most common type, with one or more bald patches.
- Alopecia totalis: loss of nearly all or all scalp hair.
- Alopecia universalis: loss of scalp hair plus body hair.
Some people have one episode and then see regrowth. Others go through cycles of shedding and regrowth for years. Alopecia areata does not like predictability, which is one reason it can be so frustrating.
How Alopecia Areata Fits Into the Bigger Hair Loss Picture
Not all hair loss is the same, and that matters. Alopecia areata is only one cause of hair loss, even though it gets a lot of attention because the bald patches can appear suddenly. Other common causes include androgenetic alopecia, also known as pattern hair loss, traction alopecia from tight hairstyles, telogen effluvium after illness or stress, thyroid problems, nutritional deficiencies, certain medications, scalp infections, and hair-pulling disorders.
That is why self-diagnosing from a bathroom mirror can be tricky. Patchy hair loss may look dramatic, but the cause is not always alopecia areata. A dermatologist can usually sort it out much faster than a late-night internet spiral and a magnifying mirror combo.
What Causes Alopecia Areata?
The short answer is autoimmunity. The longer answer is that alopecia areata seems to happen when genetics, the immune system, and environmental triggers all decide to hold a chaotic group project.
Immune System Misfire
In alopecia areata, the immune system attacks hair follicles, interrupting normal hair growth. The follicles are not destroyed in the way they are with scarring alopecias, which is why regrowth is often possible. Think of it less like a building demolition and more like the lights being switched off without warning.
Genetics and Family History
Some people with alopecia areata have a family history of the condition or of other autoimmune diseases. That does not mean you are guaranteed to develop it if it runs in the family, but it does suggest that inherited immune-system tendencies may play a role.
Other Health Conditions
People with alopecia areata may also be more likely to have related immune or allergic conditions such as thyroid disease, vitiligo, eczema, psoriasis, hay fever, or asthma. That does not mean everyone with alopecia areata has these conditions. It just means your hair may occasionally arrive with an uninvited medical subplot.
Stress and Illness
Stress does not appear to be the sole cause of alopecia areata, but many people notice hair loss after an illness, major emotional event, pregnancy, or other life stressor. In other words, stress may not write the entire script, but it can absolutely kick the door open for a flare in someone who is already vulnerable.
Common Signs and Symptoms
The classic symptom is sudden patchy hair loss. But alopecia areata is not always limited to a tidy little bald spot that politely announces itself.
- Smooth, round, or oval bald patches on the scalp or beard
- Hair loss involving eyebrows or eyelashes
- “Exclamation point” hairs that are narrower at the base
- Tingling, itching, or burning before hair falls out
- Nail changes such as pitting, roughness, or ridging
- More widespread hair loss affecting the scalp or body
For some people, the patches remain small. For others, they merge or progress. The disease can move fast, slow, or in a deeply annoying stop-and-start pattern.
How Doctors Diagnose Alopecia Areata
A dermatologist can often diagnose alopecia areata during an office visit. The diagnosis usually starts with a close look at the hair loss pattern, scalp, body hair, and nails. Many dermatologists also use a handheld magnifying tool to examine follicle openings and tiny broken hairs at the edges of bald patches.
Your doctor will usually ask about family history, recent illness, medications, autoimmune conditions, and how quickly the hair loss happened. If the diagnosis is not completely clear, they may order blood work or do a scalp biopsy to rule out other causes.
That may sound intense, but it is actually useful. A biopsy is not the default for everyone, and labs are often targeted rather than random. The goal is simple: make sure you are treating the right problem instead of throwing expensive hope at the wrong diagnosis.
Treatments for Alopecia Areata
There is currently no permanent cure for alopecia areata, but there are treatments that can help regrow hair, reduce the immune attack, and manage ongoing flares. The best treatment depends on your age, how much hair you have lost, how fast it is progressing, and how you feel about treating it at all.
Yes, that last part matters. Some people pursue aggressive treatment. Others decide to monitor, wear wigs, or use cosmetic solutions. Both approaches are valid.
1. Watchful Waiting
In mild cases, especially when there are only one or two small patches, doctors may recommend observation at first. Some people regrow hair within months without active treatment. This is the medical version of “let’s not panic yet.” It is not lazy medicine. It is recognizing that alopecia areata can sometimes reverse on its own.
2. Corticosteroids
Corticosteroids are still a standard treatment, especially for patchy alopecia areata.
- Injections: Often used for small patches on the scalp or beard. These are commonly given in the dermatologist’s office every few weeks.
- Topical steroids: Useful for children and for people who prefer to avoid injections.
- Oral steroids: Sometimes used in selected cases, though long-term use is limited by side effects.
These treatments work by calming the immune response. They can be effective, but regrowth may be temporary, and relapses can still happen.
3. Minoxidil
Minoxidil is often used as a helper rather than the star of the show. It may support regrowth and help maintain hair after other treatments start working. Dermatologists sometimes recommend it for the scalp, beard, or even eyebrows in selected cases. It is not a magic switch, but it can be a useful supporting actor.
4. Anthralin and Contact Immunotherapy
For more extensive disease, dermatologists may use treatments that intentionally irritate or redirect the immune response in the scalp. Contact immunotherapy is a long-standing option for widespread alopecia areata, though it requires regular office visits and patience. It is not exactly glamorous, but for some patients it is worth the effort.
5. JAK Inhibitors
This is where the treatment landscape has gotten much more interesting. JAK inhibitors are oral medicines that target immune signaling and can help some people with severe alopecia areata regrow substantial amounts of hair. These medications are a big reason many dermatologists are talking about alopecia areata with more optimism than they could a few years ago.
Current FDA-approved options for severe alopecia areata include:
- Baricitinib for adults with severe disease
- Ritlecitinib for adults and adolescents age 12 and older with severe disease
- Deuruxolitinib for adults with severe disease
Important reality check: these medicines are not casual over-the-counter scalp vitamins with cute labels. JAK inhibitors can carry serious risks and require medical supervision. Doctors may review infections, vaccines, lab results, liver status, cardiovascular risk, clotting risk, and other safety issues before and during treatment. They can be life-changing for some people, but they are definitely not “just pop a pill and call it a day.”
6. Other Systemic Treatments
Some doctors may use medications off-label in carefully selected patients, especially when standard therapies are not enough. These may include immunosuppressive drugs or older JAK inhibitors not specifically approved for alopecia areata. Treatment decisions here should be individualized and guided by a specialist who actually treats hair loss regularly.
7. Cosmetic and Supportive Options
Treatment is not only about follicles. It is also about daily life. Wigs, toppers, eyebrow products, false lashes, scalp powders, microblading discussions, hats, scarves, and other camouflage options can make a huge difference in comfort and confidence. These are not “giving up.” They are tools. Use them unapologetically.
Tips to Cope With Alopecia Areata Day to Day
Hair loss can be medically harmless and emotionally exhausting at the same time. Those two things can coexist. Coping well usually means treating both the physical and emotional sides of the condition.
Protect Your Scalp
Bare areas on the scalp burn more easily than people expect. Wear a hat or apply broad-spectrum sunscreen with SPF 30 or higher if your scalp is exposed. Cold weather can also hit harder when hair is missing, so scarves and warm hats are not just style choices. They are practical equipment.
Protect Your Eyes and Nose
If you lose eyebrows or eyelashes, your eyes may feel more exposed to sweat, dust, and light. Glasses, hats, and cosmetic solutions can help. If nasal hair is affected, your nose may feel drier or more sensitive to dust and air particles.
Be Gentle With Hair You Still Have
Use fragrance-free, gentle products when possible. Avoid tight hairstyles that pull on the scalp. Go easy on harsh chemicals, heat tools, and any styling routine that seems designed by a villain with a vendetta against follicles.
Get Emotional Support Early
Support groups, therapists, trusted friends, and patient communities can be incredibly helpful. You do not need to wait until you are falling apart to ask for support. Alopecia areata can affect self-esteem, work confidence, dating, school life, and social comfort. That is not vanity. That is being human.
Manage Stress Without Blaming Yourself
Stress management may help some people feel more in control, but it is not fair to treat alopecia areata as a self-help failure. Yoga, therapy, walking, sleep, meditation, journaling, and exercise can all be useful. Just do not turn wellness into another job where you also get graded by your eyebrows.
See a Dermatologist Who Knows Hair Loss
A board-certified dermatologist can help you understand what kind of hair loss you have, what is realistic to expect, and which treatments fit your goals. This matters because the internet loves overselling miracle oils, miracle vitamins, miracle scalp rollers, and other miracle-adjacent nonsense.
What Living With Alopecia Areata Often Feels Like
One of the hardest parts of alopecia areata is that it changes more than your hair. It changes your routine, your mirror habits, your social calculations, and sometimes the tone of your entire day. Many people describe the first patch as a shock. It is not always physically painful, but it can feel emotionally loud. Suddenly you are staring at a spot on your scalp that was not there last week, trying to decide whether you are overreacting, underreacting, or entering your supervillain origin story.
Then comes the uncertainty. Will it spread? Will it stop? Will it grow back? Will the regrowth stay? Alopecia areata is difficult partly because it rarely gives a clean answer. A lot of people say the unpredictability is worse than the patch itself. Hair may return in one spot while a new patch appears somewhere else, which can make progress feel oddly slippery. You think you are winning, and then your immune system sends a plot twist.
There is also the social side. People may ask invasive questions. Some mean well and still manage to say the wrong thing with Olympic precision. Others assume hair loss must be caused by stress, bad diet, poor self-care, or some mystery shampoo crime. For people who lose eyebrows or eyelashes, the change can feel especially exposing because those features affect facial expression and how “recognizable” you feel to yourself. A missing eyebrow can do more emotional damage than it has any right to.
Children and teens can have an especially tough time. School-aged kids may feel singled out, while teenagers are forced to cope during the exact life stage when appearance already feels like a public referendum. Adults are not magically protected either. Many feel awkward at work, on video calls, at the gym, on dates, or during family events. Even everyday tasks like getting ready in the morning may become emotionally loaded.
At the same time, many people gradually build a new kind of resilience. They learn which wig feels best, which hat actually stays on in wind, which eyebrow pencil deserves a medal, and which friends can sit with them without offering bizarre internet remedies involving onions. Some become more open. Some become more private. Some shave their heads and feel powerful. Some wear toppers and feel relieved. Some do both depending on the day. There is no single right emotional style for living with alopecia areata.
Another common experience is grief mixed with adaptation. People may feel embarrassed for grieving “just hair,” but hair is tied to identity, culture, routine, gender expression, and self-image. Losing it can feel like losing a familiar version of yourself. Regrowth can bring joy, but sometimes it brings anxiety too, because you start worrying about losing it again. That emotional whiplash is real.
Over time, many people say the biggest shift happens when they stop treating every hair in the sink like a breaking news event. They still care, but they are not held hostage by every strand. Support groups, therapists, experienced dermatologists, and honest conversations can help get you there. So can simple acts of control: protecting your scalp, finding cosmetics or head coverings you like, tracking flares without obsessing over them, and learning how to explain the condition in one sentence without feeling like you owe the world a TED Talk.
If there is one theme that shows up again and again, it is this: alopecia areata can be deeply disruptive, but it does not erase personality, talent, attractiveness, intelligence, humor, or worth. It may change the frame, but it does not change the person in the picture.
Final Thoughts
Alopecia areata is more than a cosmetic issue, even though the hair loss is what everyone sees first. It is an autoimmune condition with real medical, emotional, and social impact. The upside is that the field has moved forward. Dermatologists now have more tools than ever, from corticosteroids and topical therapies to newer JAK inhibitors for severe cases. At the same time, wigs, scalp care, counseling, and support communities remain just as important because treating alopecia areata is not only about regrowing hair. It is also about helping people feel like themselves again.
If you are dealing with sudden or patchy hair loss, getting a proper diagnosis is worth it. Sometimes hair grows back on its own. Sometimes it needs medical help. Sometimes the best first step is not a miracle serum but a dermatologist, a good sunscreen, and the radical decision to stop blaming yourself for something your immune system started.






