Table of Contents >> Show >> Hide
- What Are Cytotoxic Agents?
- Common Uses of Cytotoxic Agents
- How Cytotoxic Agents Help
- Main Types of Cytotoxic Agents
- How Cytotoxic Agents Are Given
- Limitations of Cytotoxic Agents
- When Cytotoxic Agents Are Still the Right Choice
- Questions Patients Should Ask
- Real-World Experiences With Cytotoxic Agents
- Final Thoughts
Cytotoxic agents sound like something pulled from a sci-fi lab where everyone wears dramatic goggles and speaks only in acronyms. In real medicine, though, they are much more practical than theatrical. These drugs are designed to kill cells or stop them from multiplying, which is exactly why they have remained such an important part of treatment for many serious diseases.
Most people hear the term in connection with cancer treatment, and that is still where cytotoxic agents are used most often. But the story does not end there. Some cytotoxic drugs are also used in lower doses to calm an overactive immune system in severe autoimmune diseases. That makes them powerful, flexible, and, yes, a little intimidating.
This is where the balance gets interesting. Cytotoxic agents can shrink tumors, reduce symptoms, lower the risk of recurrence, and sometimes help put disease into remission. At the same time, they can affect healthy cells, create side effects, and require close monitoring. In other words, they are helpful but not magical, strong but not selective, and valuable but never casual.
This guide explains what cytotoxic agents are, how they work, where they are used, and what their real limitations look like in modern care.
What Are Cytotoxic Agents?
A cytotoxic agent is a substance that kills cells. In medical practice, the term usually refers to drugs that damage or destroy rapidly dividing cells. Because cancer cells tend to grow and multiply faster than most normal cells, cytotoxic drugs have long been used to treat many kinds of cancer.
That said, “cytotoxic” is a broader idea than “chemotherapy” alone. Conventional chemotherapy drugs are the best-known cytotoxic agents, but the category can also include certain specialized cancer medicines, including some cytotoxic proteins and drug combinations designed to destroy abnormal cells. The basic idea stays the same: hit the cells that are driving disease hard enough to stop them from spreading, reproducing, or surviving.
Doctors may also use some cytotoxic medicines outside oncology. For example, methotrexate and cyclophosphamide can be used in selected autoimmune conditions when the immune system is attacking the body’s own tissues. In that setting, the goal is not to blast a tumor but to suppress destructive cell activity and reduce inflammation before it causes lasting damage.
So while the label sounds technical, the concept is simple. Cytotoxic agents are cell-killing or cell-stopping drugs used when the disease itself is dangerous enough that a strong medical response is necessary.
Common Uses of Cytotoxic Agents
Cancer treatment
This is the main arena. Cytotoxic agents are used to treat blood cancers such as leukemia, lymphoma, and multiple myeloma, as well as many solid tumors, including cancers of the breast, lung, ovary, colon, and more. They may be used alone, but they are often combined with surgery, radiation, hormone therapy, targeted therapy, or immunotherapy.
Doctors use them in several ways. They may be given as the main treatment to kill cancer cells directly. They may be used before surgery or radiation to shrink a tumor, which is often called neoadjuvant therapy. They may also be used after surgery to destroy microscopic cancer cells left behind, which is called adjuvant therapy. In advanced disease, they may help control cancer growth, reduce pain, and improve quality of life.
Conditioning before stem cell transplant
Some cytotoxic regimens are used before bone marrow or stem cell transplant. In this setting, the drugs help wipe out diseased marrow cells and make room for healthy replacement cells. It is an intense use of an already intense drug category, which tells you a lot about how powerful these medicines can be.
Autoimmune and inflammatory diseases
In lower or carefully adjusted doses, certain cytotoxic drugs may be used to treat diseases such as severe vasculitis, lupus, psoriasis, rheumatoid arthritis, and some lung conditions linked to autoimmune damage. The purpose here is to slow harmful immune activity, protect organs, and prevent long-term tissue injury.
This can be especially important when inflammation is threatening the kidneys, lungs, blood vessels, skin, or nervous system. In those cases, the medication may be aggressive because the disease is aggressive. Medicine loves balance, but it is not afraid of a heavyweight match when needed.
How Cytotoxic Agents Help
They interfere with cell growth
Cytotoxic agents help by disrupting the machinery cells need to survive and reproduce. Some damage DNA directly. Some interfere with the building blocks cells use to make DNA or RNA. Others stop cells during the process of division, which prevents them from creating new copies. If a cell cannot copy itself properly, it cannot keep the disease moving forward.
They work throughout the body
One major advantage of many cytotoxic drugs is that they circulate systemically. That means they travel through the bloodstream and can reach cancer cells beyond the main tumor site. This matters when disease has spread, when stray cells are too small to see on a scan, or when doctors want to reduce the chance of recurrence after surgery.
They can shrink tumors and relieve symptoms
For many patients, the benefit is not just theoretical or microscopic. Tumors can shrink. Pressure on nearby tissues can decrease. Pain, bleeding, bowel obstruction, and other symptoms may improve. Even when a cure is not possible, cytotoxic therapy can still have a meaningful job to do.
They can be combined for greater effect
Different cytotoxic drugs attack cells in different ways, which is why many treatment plans use combination regimens. One drug may damage DNA while another blocks replication or division. Together, they can make it harder for abnormal cells to survive. Combination therapy also helps address the reality that cancer is rarely one-note. It is more like a bad band with too many instruments, so treatment often needs more than one way to break up the show.
Main Types of Cytotoxic Agents
There are several major classes of cytotoxic drugs, and each works a little differently.
Alkylating agents and platinum-based drugs
These drugs damage DNA so cells cannot reproduce normally. They are widely used across many cancers. Examples include cyclophosphamide, cisplatin, carboplatin, oxaliplatin, and ifosfamide. They are effective, but they can also affect bone marrow and other normal tissues.
Antimetabolites
These drugs act like fake building blocks for DNA or RNA. Cancer cells try to use them, and the copying process breaks down. Examples include methotrexate, 5-fluorouracil, capecitabine, gemcitabine, and cytarabine. These agents are especially important in many leukemias and solid tumors.
Anthracyclines and other antitumor antibiotics
These medicines interfere with DNA and the enzymes cells use to copy it. Doxorubicin is one of the best-known examples. They can be highly effective, but some have lifetime dose limits because of the risk of heart damage.
Topoisomerase inhibitors
These block enzymes that help unwind and copy DNA. If the DNA cannot be handled properly, the cell cannot keep dividing. Irinotecan, topotecan, and etoposide fall into this family.
Mitotic inhibitors
These drugs stop cells during division. Taxanes and vinca alkaloids are classic examples. Paclitaxel, docetaxel, and vincristine are widely used, but they can also cause nerve-related side effects in some people.
Cytotoxic agents used in immune disease
Some drugs overlap oncology and autoimmune care. Methotrexate is a prime example. In cancer, it can act as an antimetabolite that slows abnormal cell growth. In autoimmune disease, lower-dose methotrexate can help reduce inflammation and prevent damage to joints, skin, or organs. Cyclophosphamide is another crossover drug, especially in severe autoimmune disease affecting vital organs.
How Cytotoxic Agents Are Given
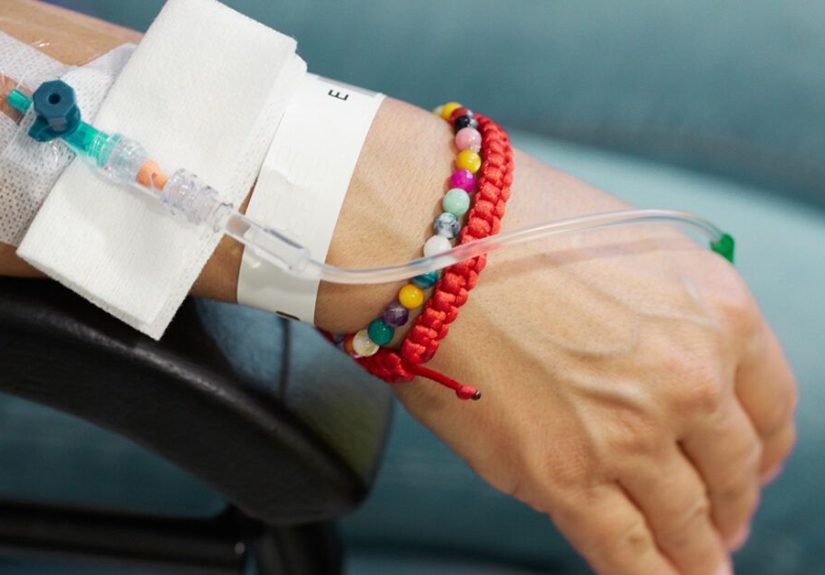
Cytotoxic medicines can be delivered in several ways. Some are given by intravenous infusion, some by injection, and some by mouth as pills or capsules. A few are delivered in more specialized ways, such as into the spinal fluid for certain cancers.
Treatment is usually given in cycles. A cycle may involve one day of treatment, several treatment days, or a series of doses followed by a rest period. That pause is not a scheduling quirk. It exists so the body has time to recover, especially healthy tissues like bone marrow, the digestive lining, and hair follicles.
The exact schedule depends on the disease, the specific drug, the dose, the patient’s overall health, and how well the body tolerates treatment. This is why two people can both say, “I’m on chemo,” and still be having wildly different weeks.
Limitations of Cytotoxic Agents
They are not highly selective
The biggest limitation is built into the mechanism. Cytotoxic drugs target cells that grow and divide quickly, but cancer cells are not the only cells in the body that do that. Hair follicles, cells lining the mouth and intestines, reproductive tissues, and blood-forming cells in the bone marrow can all be affected too. That is why side effects are so common.
Side effects can be significant
Common side effects may include fatigue, nausea, vomiting, appetite loss, mouth sores, diarrhea or constipation, hair loss, low blood cell counts, greater risk of infection, anemia, easy bruising, and nerve problems such as numbness or tingling. Depending on the drug, some people may also have fertility concerns, heart toxicity, kidney problems, lung injury, or long-term complications that show up after treatment ends.
Not every patient gets every side effect, and modern supportive care has improved dramatically. Antinausea medicines, growth factor support, dose adjustments, hydration plans, and closer monitoring all help. Still, the side-effect profile remains one of the main reasons cytotoxic therapy must be individualized.
Some cancers resist treatment
Another limitation is resistance. Cancer cells can adapt. They may repair DNA damage more effectively, pump drugs out of the cell, change the target the drug was supposed to hit, or activate backup survival pathways. When that happens, a treatment that once worked may work less well over time.
They may not be the best fit for every cancer
Some tumors respond beautifully to cytotoxic agents. Others do not. In many cancers today, targeted therapy, hormone therapy, immunotherapy, or antibody-based treatment may offer better results, fewer side effects, or both, especially when a tumor has a known molecular target. In practice, cytotoxic therapy is still essential, but it is no longer the only major player on the field.
Monitoring is not optional
These drugs require lab tests, symptom tracking, and regular follow-up. Blood counts may need close monitoring. Kidney or liver function may have to be checked. Heart testing may be needed for some medicines. Dose changes are common because treatment has to match the patient, not just the disease.
Safety matters beyond the patient
Cytotoxic agents can also be hazardous for healthcare workers, caregivers, and family members if handled improperly. Drug residue and body fluids may require special precautions for a period after treatment. That does not mean panic; it means good instructions matter.
When Cytotoxic Agents Are Still the Right Choice
With all these limitations, you might wonder why cytotoxic agents remain so widely used. The answer is simple: because they still work. For many cancers, they are proven, accessible, and effective. They can cure some diseases, deepen remission, improve survival, and make surgery or radiation more successful. In autoimmune disease, they can sometimes prevent irreversible organ damage when milder options are not enough.
Modern treatment does not usually frame cytotoxic drugs as “old” and everything else as “better.” Instead, clinicians look at what fits the biology of the disease, the treatment goal, and the patient’s overall situation. Sometimes the best plan is a classic cytotoxic regimen. Sometimes it is a combination of chemotherapy and newer targeted or immune-based drugs. Sometimes it is a lower-dose immune-modulating approach for a noncancer illness. The real question is not whether a drug sounds modern. The real question is whether it gives the patient the best chance at benefit with an acceptable level of risk.
Questions Patients Should Ask
If a doctor recommends a cytotoxic agent, helpful questions include: What is the goal of treatment? Is it curative, preventive, or palliative? Why is this drug being chosen over other options? What short-term and long-term side effects matter most for this specific regimen? How will my labs and organ function be monitored? What symptoms should make me call right away? Are there fertility, pregnancy, infection, or home-safety concerns I need to plan for?
Those questions are not dramatic. They are smart. And when the drug category is this powerful, smart is a very good place to start.
Real-World Experiences With Cytotoxic Agents
Reading about cytotoxic agents in a clean medical summary is one thing. Living with them is another. The real-world experience often starts with information overload: new terms, new schedules, consent forms, lab numbers, infusion appointments, and a growing suspicion that your calendar now belongs to somebody else. Many patients say the hardest part at first is not even the medicine itself. It is the uncertainty of not knowing how their body will react.
For people receiving cytotoxic chemotherapy for cancer, the treatment rhythm can become part of daily life. There may be infusion days, recovery days, and a stretch of time when energy slowly returns before the next cycle begins. Some people feel tired almost immediately. Others are fine on treatment day and get hit later like a delayed weather system. Fatigue is often described not as ordinary tiredness but as a heavier, stranger exhaustion that does not fully respond to rest.
Food can become unexpectedly complicated. A favorite meal may suddenly taste metallic, bland, or just plain wrong. Some people deal with nausea. Others struggle more with mouth sores, bowel changes, or poor appetite. A common experience is having to rethink routine habits, from what time to eat to how much water to drink to which snacks are easiest when nothing sounds appealing. It is not glamorous, but symptom management often becomes a full-time side project.
Hair loss, when it happens, can be emotionally bigger than outsiders realize. Patients may understand perfectly well that hair grows back, yet still feel shocked by the speed and visibility of the change. For some, it affects privacy, identity, and social confidence. For others, it is less upsetting than the fatigue or neuropathy. The point is that the lived experience is deeply personal. The same regimen can feel like a mild interruption to one person and a major life rewrite to another.
People taking cytotoxic agents for autoimmune disease may have a different path, but many of the same themes appear. There is often relief that a serious medication exists, mixed with anxiety about what it could do. Patients may feel caught between two truths: the disease itself is dangerous, and the treatment is serious. When drugs like methotrexate or cyclophosphamide begin to work, some people notice less pain, less swelling, better breathing, or improved lab results before they fully “feel better.” That gap between medical improvement and lived improvement can be frustrating.
Caregivers also have their own experience. They often become part scheduler, part pharmacist, part emotional support team, and part detective watching for fever, dehydration, confusion, or a symptom that suddenly matters more than it did yesterday. Families may need to learn practical safety steps at home, especially after chemotherapy, because body fluids can contain drug waste for a short time after treatment.
Then there is the emotional layer. Many people say the treatment experience teaches them to think in shorter time frames. Instead of asking, “How will this year go?” they ask, “How do I get through this week?” That mindset is not weakness. It is adaptation. Cytotoxic therapy can be physically demanding, but it can also reveal how flexible people become when they have to be. A good care team, clear instructions, symptom reporting, and realistic expectations often make the experience safer and more manageable.
Final Thoughts
Cytotoxic agents remain one of the most important tools in serious disease treatment because they can directly stop or kill harmful cells. They are used most often in cancer care, but they also play a role in selected autoimmune and inflammatory diseases. Their strength lies in their ability to interfere with cell growth, reach disease throughout the body, and work in combination with other therapies.
The catch is equally important: these drugs are powerful because they are not perfectly selective. Healthy fast-growing cells can be damaged too, which is why side effects, monitoring, and individualized treatment plans matter so much. Cytotoxic agents are neither miracle cures nor outdated relics. They are high-impact medicines with real benefits, real burdens, and a continuing role in modern care.
When used thoughtfully, they can save lives, preserve organ function, and improve quality of life. When misunderstood, they can sound scarier or simpler than they really are. The truth, as usual, lives in the middle: cytotoxic agents are serious drugs used for serious problems, and in the right setting, they can make a very real difference.






