Table of Contents >> Show >> Hide
- Why the “400% Higher” Headline Exists
- Ozempic and Wegovy Are Cousins, Not Twins
- Why the U.S. Pays So Much More
- What Patients Actually Pay at the Pharmacy
- The Coverage Problem Is Bigger Than the Drug Itself
- Policy Pressure Is Finally Building
- Why This Story Matters Beyond Weight Loss Headlines
- Experiences Patients and Families Commonly Describe
- Conclusion
- SEO Tags
In America, even a tiny injection pen can come with a jumbo-sized price tag. That is the uncomfortable truth behind Ozempic and Wegovy, two blockbuster semaglutide drugs that have become household names, punchlines, policy flashpoints, and, for many patients, serious financial headaches. Depending on which country you compare them to, the U.S. price of these drugs can be nearly four times higher or more than five times higher. In plain English, that means Americans can end up facing prices that are roughly 300% to 400%-plus higher than what patients in other wealthy nations see on paper.
That headline gets attention because it sounds outrageous, and frankly, it is. But the real story is even messier. The U.S. list price is not always what insured patients pay. Coupons, rebates, direct-to-patient programs, prior authorization rules, deductibles, and benefit exclusions all crash into one another like shopping carts with a grudge. One patient may pay $25. Another may pay hundreds every month. Another may discover that “covered” and “affordable” are not even close to being synonyms.
So yes, Ozempic and Wegovy are expensive in the United States. But the deeper question is why they are so expensive, who actually feels the pain, and what the pricing drama reveals about the broader American healthcare machine. Spoiler: the machine does not exactly run on simplicity.
Why the “400% Higher” Headline Exists
The headline is rooted in international price comparisons that have embarrassed the U.S. system in broad daylight. A well-known analysis comparing U.S. prices with peer countries found that Ozempic was priced at more than five times the U.S. price in Japan, while Wegovy was nearly four times the U.S. price in Germany. That is where the “400% higher” framing comes from. It is not marketing drama. It is math with attitude.
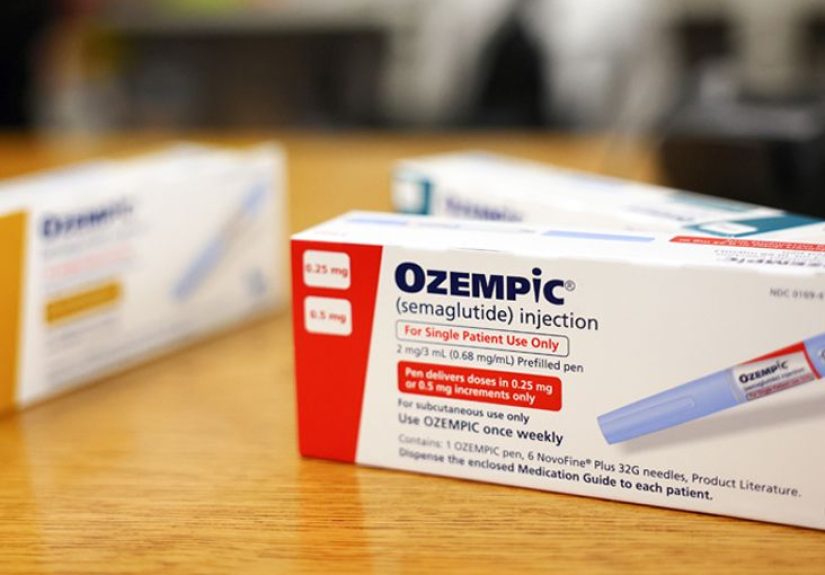
Still, it helps to understand what is being compared. Most of these international comparisons use list price, also known as wholesale acquisition cost. Think of list price as the sticker price on a car nobody actually wants to pay, except this is healthcare, so sometimes people do get stuck paying something painfully close to it. In the U.S., Ozempic’s current list price is about $1,027.51 per package, while Wegovy’s current list price is about $1,349.02 for a month’s supply. Those numbers are high enough to make even a healthy wallet feel faint.
And yet list price is only the beginning of the story. U.S. drug pricing has layers. Some are visible. Some are hidden. Some seem to have been invented by people who think clarity is overrated. Pharmacy benefit managers negotiate rebates. Insurers decide formularies. Employers decide whether weight-loss drugs are covered. Government programs apply their own rules. Manufacturers offer savings cards and self-pay channels. The result is a system where the official price can look sky-high, but the checkout price varies wildly depending on who you are, what plan you have, and whether you had the bad luck to ask the wrong pharmacy on the wrong day.
Ozempic and Wegovy Are Cousins, Not Twins
Same active ingredient, different labels
Ozempic and Wegovy are both semaglutide products made by Novo Nordisk, but they are not interchangeable from a regulatory and insurance standpoint. Ozempic is widely associated with type 2 diabetes treatment, while Wegovy is marketed for chronic weight management and also carries a cardiovascular risk-reduction indication for certain adults. That distinction matters because insurance plans do not just look at the molecule. They look at the label, the diagnosis code, the benefit category, and sometimes, it seems, the alignment of the moon.
This is one reason pricing feels so strange to patients. Two drugs can share a core ingredient, yet they travel through different reimbursement pathways. One may be easier to cover under a diabetes benefit. The other may face exclusions because many health plans have historically treated anti-obesity drugs as optional, expensive, or politically inconvenient. That is changing, but slowly, and slowly is not a comforting word when your refill is due next Tuesday.
Why Wegovy often feels more expensive
Wegovy’s list price has long drawn particular attention because obesity treatment coverage in the U.S. has lagged far behind clinical demand. If a patient has strong insurance coverage for diabetes medications, Ozempic may feel reachable. If a patient seeks treatment primarily for obesity, Wegovy can feel like a VIP product with a velvet rope and no mercy. Even when the clinical case is compelling, coverage rules can force patients into appeals, prior authorizations, step therapy, or outright denials.
That is changing at the edges. Wegovy’s heart-risk-reduction indication opened the door to broader coverage for some patients, including millions of Medicare beneficiaries who may qualify under that narrower clinical path. But “broader coverage” is not the same as “easy access.” It just means the maze got a few more exits.
Why the U.S. Pays So Much More
The U.S. does not negotiate drug prices the way peer nations do
Many wealthy countries use national systems, centralized negotiations, or direct price controls to hold down prescription drug costs. The U.S. generally does not. American pricing is more fragmented, more commercial, and more tolerant of large spreads between list price and net price. Drugmakers argue that the U.S. market rewards innovation. Critics argue that it rewards invoices with superhero powers. Both perspectives can be heard at every policy hearing where semaglutide prices come up.
In countries with stronger pricing controls, the government or a central payer can push back with one loud, unified voice. In the U.S., the pushback is scattered across private insurers, PBMs, employers, state Medicaid programs, federal programs, and cash-paying patients. That fragmentation weakens negotiating power and allows list prices to stay elevated.
Rebates distort the picture
Another reason U.S. prices look bizarre is that the list price is not necessarily the final price that flows through the system. Manufacturers may pay substantial rebates to PBMs and insurers in exchange for better formulary placement. That means the list price can stay high while the net price paid by large intermediaries falls lower behind the curtain.
The problem is that patients do not always benefit equally from those hidden discounts. If your coinsurance is based on the list price, or if you have not met your deductible, the rebate drama happening backstage does not feel helpful. You are still standing at the front of the theater being asked to buy a very expensive ticket.
Demand exploded, and pricing power came with it
Semaglutide is not just another prescription category. These drugs sit at the intersection of diabetes care, obesity medicine, cardiometabolic health, employer benefit strategy, telehealth expansion, celebrity culture, and social media obsession. Demand surged because the clinical results were meaningful and highly visible. When demand is intense and supply is constrained or newly expanding, pricing power tends to stay with the manufacturer unless competition or regulation forces the issue.
That helps explain why these drugs became symbols in a national fight over affordability. They are not obscure therapies used by a tiny population. They are mainstream enough that nearly everyone knows someone who has asked about them, tried them, or argued about them at brunch.
What Patients Actually Pay at the Pharmacy
Here is where the story gets tricky. A patient with strong commercial insurance may pay very little for Ozempic or Wegovy if the drug is covered and the patient qualifies for manufacturer savings. Some eligible patients can bring out-of-pocket costs down dramatically. For others, self-pay or direct-purchase channels can reduce monthly costs to a few hundred dollars instead of the full list price.
But “dramatically lower than terrible” is not the same as “cheap.” A cash price in the low hundreds still adds up fast over a year. For a chronic therapy, even a discounted monthly cost can feel like a second utility bill that never stops arriving. And for patients whose plans exclude obesity drugs, or whose coinsurance is pegged to a high list price, the burden can still be brutal.
GoodRx and manufacturer programs illustrate the tension perfectly. Official list prices remain above $1,000 a month, but discount pathways can bring some Ozempic fills to around $349 or $499 depending on dose and channel, while some Wegovy offers have pushed certain doses into a lower few-hundred-dollar range. That sounds better, because it is better. It just is not exactly normal. The system is basically saying, “Congratulations, you do not have to pay the absurd price. You may instead pay the merely painful price.”
And even those lower pathways come with fine print. Eligibility rules apply. Government beneficiaries are often excluded from certain savings offers. Some pricing is limited to specific channels, doses, or time periods. A patient can spend an afternoon trying to decode coverage, coupon rules, and pharmacy inventory only to end the day feeling like they accidentally majored in pharmaceutical bureaucracy.
The Coverage Problem Is Bigger Than the Drug Itself
America’s obesity burden is enormous. Recent CDC data show that adult obesity prevalence remains above 40%, which means the clinical need for effective treatment is not some fringe conversation. It is central to public health. Yet insurance coverage has not kept pace with that reality. Medicaid coverage for obesity-focused GLP-1 drugs remains limited in many states, and employer plans vary widely. Some cover these medications generously. Some cover them reluctantly. Some pretend obesity treatment is a lifestyle choice with a billing code problem.
This mismatch creates a bizarre market. The country has a large clinical need, strong patient demand, and serious evidence supporting treatment for some people, but access still depends heavily on the fine print of benefit design. The result is a treatment category that is medically important but financially unstable for many families.
That instability also creates inequality. Patients with comprehensive employer-sponsored insurance, flexible income, and time to fight denials are in a stronger position than patients with high deductibles, limited savings, or fragmented coverage. In theory, medicine should follow clinical need. In practice, it often follows the insurance map.
Policy Pressure Is Finally Building
The political heat around Ozempic and Wegovy pricing is no longer subtle. Congressional scrutiny has increased. The Senate has publicly challenged the pricing of these drugs. Medicare price-negotiation policy is reshaping expectations for future access and affordability. Novo Nordisk has already announced that it plans to lower the U.S. list price of Wegovy and Ozempic to $675 effective January 1, 2027.
That announced cut matters for two reasons. First, it is an acknowledgment that the old list-price structure became hard to defend. Second, it shows that public pressure, policy change, and market competition can move even giant products. But it also highlights how strange the system has been all along. If a list price can be cut so sharply and the market still functions, people naturally ask the obvious question: why was the earlier price allowed to sit there like a luxury chandelier for so long?
Even so, a future list-price reduction does not magically solve today’s access issues. Coverage rules will still matter. Benefit exclusions will still matter. Prior authorization will still matter. And because U.S. healthcare loves complexity the way toddlers love glitter, simplification may remain in short supply.
Why This Story Matters Beyond Weight Loss Headlines
It is easy to reduce Ozempic and Wegovy to celebrity gossip, social media before-and-after photos, or another round of internet arguments about vanity versus medicine. That misses the point. These drugs sit at the center of a much larger debate about how America values treatment, who gets access to modern therapies, and whether a clinically useful medicine can become functionally out of reach because the pricing system behaves like a carnival game.
For people with type 2 diabetes, obesity, or cardiovascular risk, this is not abstract. High prices influence whether patients start treatment, stay on treatment, or stop treatment. They affect household budgets, employer benefits, Medicaid spending, and long-term health outcomes. When a drug works but the price is unstable, the treatment journey becomes financially exhausting even before the side effects enter the chat.
The bigger lesson is not just that America pays more. It is that America often pays more while making the buying process harder to understand. That combination is what frustrates patients most. A high price is bad enough. A high price wrapped in confusion is a special kind of insult.
Experiences Patients and Families Commonly Describe
A common experience begins with optimism. A patient hears that Ozempic or Wegovy may help with blood sugar control, weight management, or heart-risk reduction. The doctor agrees it could be clinically appropriate. The patient leaves the appointment relieved, maybe even excited, thinking modern medicine has finally handed over something useful. Then the pharmacy runs the claim, and the mood changes fast. Suddenly there is a deductible issue, a prior authorization request, a quantity limit, or a message that the drug is “not covered for this indication.” In less than five minutes, hope turns into paperwork.
Another familiar experience is the deductible reset. A patient may have managed to afford the medication late in the previous year, only to get slammed in January when the plan resets and out-of-pocket costs jump again. Nothing about the medication changed. Nothing about the medical need changed. Only the calendar changed. Yet the bill behaves like it joined a gym over the holidays and came back stronger.
Then there is the confusion around “covered” status. Patients often assume that if a drug is on the formulary, access will be straightforward. Not necessarily. It may be covered only after step therapy. It may be covered only for diabetes, not obesity. It may require proof of body mass index, proof of failed prior treatments, proof of a specific diagnosis, or proof that the patient is willing to spend half a workday on hold. The word “covered” can mean many things in American healthcare, and some of them are less comforting than advertised.
Families also describe the emotional whiplash of comparing prices. One person with employer coverage pays very little. Another person, with a different employer or no obesity-drug coverage, sees a bill that feels closer to rent than routine care. Two patients can sit in the same waiting room, receive similar prescriptions, and walk into completely different financial realities. That inconsistency erodes trust because it makes the system feel arbitrary, even when the fine print technically explains it.
Medicare beneficiaries have their own version of the maze. Some became newly hopeful when Wegovy’s cardiovascular indication expanded the possibility of coverage for certain patients. But hope still has to survive operational reality. Eligibility must match the label. Plans must process the claim properly. Physicians may need to document the right condition in the right way. Patients who hear “this may now be covered” often discover that “may” is carrying a lot of weight in that sentence.
Even people who eventually get access often describe a background hum of anxiety. Will the coupon still work next month? Will the pharmacy have the dose in stock? Will the insurer suddenly require a new authorization? Will the out-of-pocket price jump after a plan change? That uncertainty matters. Long-term treatment is easier when patients can predict the cost. A lower but unstable price can still be stressful because households budget better with consistency than with cliff edges.
There is also a quieter group in this story: patients with diabetes who feel as though the internet turned their medication into a cultural spectacle. They may rely on Ozempic for a medically necessary reason, yet still encounter side-eye, supply worries, or assumptions driven by media chatter. For them, the pricing debate is not just about affordability. It is about whether a useful chronic medication can remain reliably accessible when it becomes famous.
All of these experiences point to the same conclusion. The problem is not simply that semaglutide drugs are expensive. It is that the path from prescription to possession is unstable, confusing, and uneven. Patients can handle hard news better than mixed signals. What wears them down is the combination of high prices, inconsistent coverage, and endless rules that seem designed to turn a pharmacy counter into an escape room.
Conclusion
Ozempic and Wegovy are not just expensive drugs. They are a case study in how the U.S. prescription market turns medical demand into pricing drama. International comparisons make the problem look shocking, and they should. Americans really can face prices that are several times higher than those in peer nations. But the deeper issue is not just the number on the invoice. It is the maze surrounding it.
The U.S. system allows list prices to stay high, hides discounts behind opaque negotiations, and pushes patients into wildly different out-of-pocket experiences based on insurance design rather than clinical need. That is why this debate keeps growing. It is not only about semaglutide. It is about whether a country can claim to lead in medical innovation while making access feel like a scavenger hunt with a credit check.
If future price cuts, broader coverage, and policy pressure continue, the story may improve. But for now, the lesson is simple: when Americans talk about the price of Ozempic and Wegovy, they are really talking about the price of living inside the U.S. healthcare system itself. And that, unfortunately, is where the premium really kicks in.