Table of Contents >> Show >> Hide
- What Is the Liver?
- Liver Anatomy: Where It Is and How It Is Built
- What Does the Liver Do?
- Common Symptoms of Liver Problems
- Conditions That Commonly Affect the Liver
- How Doctors Diagnose Liver Disease
- Treatment, Prevention, and Daily Care
- When Symptoms Need Prompt Medical Attention
- Real-Life Experiences Related to Liver Health
- Final Thoughts
The liver is one of those organs that quietly handles the chaos while asking for almost no applause. It does not post motivational quotes. It does not ring a bell when it saves the day. It just keeps filtering, storing, processing, producing, and balancing like the overachiever of the human body. If your organs had yearbook superlatives, the liver would win “Most Likely to Be Doing Absolutely Everything.”
That matters because the liver is not a niche organ with a tiny side quest. It is a major control center for digestion, energy use, blood chemistry, and waste processing. When it becomes inflamed, scarred, or overloaded, the body often feels the effects in ways that range from subtle fatigue to unmistakable warning signs like jaundice, swelling, itching, and confusion. The tricky part is that liver problems can also be surprisingly quiet at first.
This guide breaks down what the liver is, where it sits, how it is built, what it does, which symptoms deserve attention, what can go wrong, how doctors evaluate liver problems, and what people often experience in real life when liver health becomes part of the conversation.
What Is the Liver?
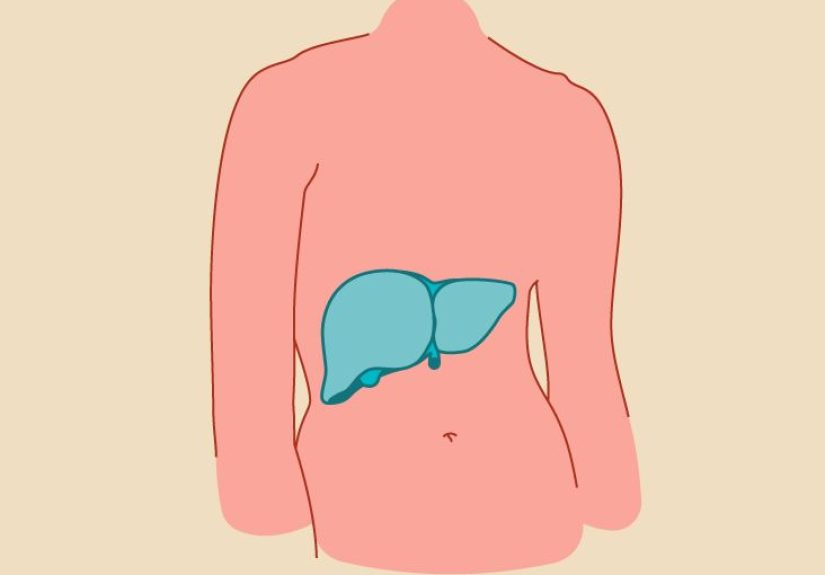
The liver is the largest internal organ in the human body. In simple terms, it is a large, reddish-brown organ that sits mostly in the upper right part of the abdomen, tucked beneath the diaphragm and resting above parts of the stomach, intestines, and right kidney. In adults, it weighs about three pounds, which is impressive for an organ that still manages to fit in without demanding designer luggage.
A basic definition of the liver is this: it is a metabolically active organ that helps process nutrients, filter blood, make bile, break down medications and toxins, support immune activity, and keep key chemical levels in balance. That is the short version. The longer version is that the liver performs hundreds of vital tasks every day, many of them so essential that even small declines in function can affect the whole body.
Liver Anatomy: Where It Is and How It Is Built
From an anatomy standpoint, the liver sits in the right upper quadrant of the abdomen. It has two main lobes and a highly organized internal structure made up of smaller working units called lobules. These tiny units help the liver carry out its endless list of chemical jobs efficiently.
One of the most interesting things about liver anatomy is its blood supply. The liver receives blood from two major sources: the hepatic artery, which brings in oxygen-rich blood, and the portal vein, which carries nutrient-rich blood from the stomach and intestines. That means the liver is strategically positioned to inspect what you eat, what you absorb, and what your body needs to store, modify, or remove.
The liver is also connected to the biliary system. It makes bile, a digestive fluid that helps the body break down and absorb fats. Bile travels through small ducts that eventually connect to larger ducts and move bile toward the gallbladder and the first part of the small intestine. In other words, the liver is not working solo. It is part of a tightly coordinated digestive and metabolic team.
What Does the Liver Do?
Asking what the liver does is a little like asking what the internet does. The answer is: a lot, and probably more than you realized. The liver helps regulate the chemical composition of the blood and supports digestion, energy storage, detoxification, and protein production.
Key liver functions include:
- Producing bile to help digest and absorb fats
- Processing nutrients absorbed from food
- Storing energy in the form of glycogen
- Helping regulate blood sugar levels
- Breaking down medications, alcohol, and other substances
- Removing waste products and helping the body clear toxins
- Making important proteins, including some involved in clotting
- Helping manage bilirubin, cholesterol, and other blood components
- Supporting immune defense by filtering substances coming from the gut
Because the liver handles so many jobs at once, problems can show up in different ways. One person may notice fatigue and stomach discomfort. Another may have abnormal blood work but no symptoms at all. Another may not realize anything is wrong until swelling, jaundice, or confusion appears. The liver does not always announce trouble with fireworks.
Common Symptoms of Liver Problems
Liver symptoms vary depending on the cause, how long the problem has been developing, and whether scarring or complications are present. Early disease may be silent. That quiet phase is one reason routine labs sometimes uncover liver trouble before a person feels sick.
Early or common symptoms may include:
- Fatigue or unusual tiredness
- Upper right abdominal pain or discomfort
- Nausea or poor appetite
- Feeling generally unwell
- Mild weight loss
More noticeable symptoms can include:
- Jaundice, or yellowing of the skin and eyes
- Dark urine
- Pale, light, or clay-colored stools
- Itchy skin
- Easy bruising or bleeding
- Swelling in the legs, ankles, or abdomen
- Abdominal fullness from fluid buildup
- Weakness and muscle loss
- Confusion, sleep changes, poor concentration, or memory problems in advanced disease
Some of these signs happen because the liver is not processing bilirubin properly. Others happen because bile flow is blocked or slowed. Still others show up when scarring changes blood flow through the liver, leading to pressure changes, fluid retention, and complications such as ascites or varices. In advanced disease, the brain can also be affected when substances that are normally cleared by the liver build up in the bloodstream.
Conditions That Commonly Affect the Liver
“Liver disease” is not one single diagnosis. It is a broad category that includes infections, inflammation, fat buildup, scarring, inherited disorders, autoimmune conditions, bile duct problems, medication-related injuries, and cancer.
Viral hepatitis
Hepatitis means inflammation of the liver. Viral hepatitis includes hepatitis A, B, and C, among others. Symptoms may include fatigue, nausea, stomach pain, dark urine, joint pain, and jaundice, but some people have few or no symptoms, especially early on. Chronic viral hepatitis can take years or even decades to become obvious.
Alcohol-associated liver disease
Long-term heavy alcohol use can injure liver cells and lead to inflammation, fatty change, fibrosis, and eventually cirrhosis. Early symptoms may be vague, which is one reason the condition can progress before people realize how much damage has occurred.
Fatty liver disease, now often called MASLD
Metabolic dysfunction-associated steatotic liver disease, or MASLD, is the modern name for what many people still know as nonalcoholic fatty liver disease. It involves extra fat accumulating in the liver and is often linked with excess body fat, type 2 diabetes, high cholesterol, high triglycerides, or broader metabolic syndrome. A more inflammatory form is called MASH. Many people with MASLD have no symptoms, which is rude but medically common.
Fibrosis and cirrhosis
Ongoing liver injury can lead to fibrosis, which means scar tissue is replacing healthy tissue. When scarring becomes severe and widespread, the condition is called cirrhosis. Cirrhosis can interfere with blood flow, liver function, and bile movement. Complications may include ascites, portal hypertension, varices, encephalopathy, bleeding problems, and liver cancer.
Inherited and autoimmune disorders
Some liver diseases are genetic, such as hemochromatosis or Wilson disease. Others are autoimmune, meaning the immune system mistakenly attacks liver tissue. Drug-induced liver injury and toxic hepatitis are additional possibilities, especially when medications, supplements, or chemicals damage the liver.
How Doctors Diagnose Liver Disease
Doctors do not diagnose liver problems from one symptom alone. Evaluation usually combines medical history, physical examination, laboratory testing, and imaging.
Common tests include:
- Blood tests: These may look at liver enzymes, bilirubin, proteins, and other markers of liver function or injury.
- Imaging: Ultrasound, CT scans, MRI, and elastography can help identify inflammation, fat buildup, enlargement, masses, or scarring.
- Fibrosis scoring tools: Some blood-test-based calculations help estimate the likelihood of advanced scarring.
- Liver biopsy: In selected cases, a small sample of liver tissue is examined for a more precise diagnosis.
Diagnosis also depends on context. For example, a person with obesity, diabetes, and mildly abnormal liver enzymes may be evaluated differently from someone who has jaundice after taking a new medication, or someone with risk factors for viral hepatitis. Liver disease is a category, not a copy-and-paste template.
Treatment, Prevention, and Daily Care
Treatment depends on the cause. Some liver conditions improve when the underlying trigger is removed. Others require long-term monitoring, medication, specialty care, or advanced interventions. In severe end-stage disease, liver transplant may be considered.
General treatment strategies may include:
- Treating viral infections when present
- Stopping alcohol use when alcohol is contributing to injury
- Managing weight, blood sugar, cholesterol, and triglycerides in metabolic liver disease
- Reviewing medications and supplements for potential liver toxicity
- Monitoring for complications such as ascites, bleeding risk, and encephalopathy
- Regular follow-up with a primary care clinician, gastroenterologist, or hepatologist
Smart ways to support liver health
- Get vaccinated against hepatitis A and hepatitis B if recommended
- Practice safer sex and avoid sharing needles or blood-contact items
- Limit or avoid alcohol
- Use medications exactly as directed
- Be cautious with supplements and “detox” products that promise miracles
- Maintain a healthy weight and stay active
- Manage diabetes, blood pressure, and cholesterol
The phrase “liver detox” gets tossed around online like confetti at a parade, but the liver is already the body’s detox expert. What it really needs is not a trendy tea with a dramatic label. It needs fewer harmful exposures, steady metabolic support, and timely medical care when something is off.
When Symptoms Need Prompt Medical Attention
Some liver-related symptoms should not be brushed off or endlessly explained away by blaming “something I ate.” Get prompt medical attention if you develop yellowing of the skin or eyes, severe abdominal swelling, vomiting blood, black tarry stools, new confusion, intense weakness, or rapidly worsening symptoms. These can point to significant liver dysfunction or serious complications.
Real-Life Experiences Related to Liver Health
One of the most frustrating parts of liver disease is how ordinary the early experience can feel. Many people expect a major organ problem to arrive with cinematic drama. Instead, it may begin with being tired all the time, feeling vaguely nauseated, noticing that appetite is off, or having a dull ache in the upper abdomen that seems too minor to mention. People often describe months of thinking they were just stressed, overworked, aging, sleeping badly, or eating poorly. Then routine blood work shows elevated liver enzymes, and suddenly the conversation changes.
Another common experience is surprise. A person goes in for a yearly checkup, or maybe for diabetes follow-up or cholesterol management, and learns they may have fatty liver disease. They were not doubled over in pain. They were still going to work, picking up groceries, forgetting to water the plants, and living a normal life. That silent quality is why liver conditions can feel emotionally strange. It is hard to process the idea that something important is wrong when your body did not send a louder memo.
For people who do develop symptoms, fatigue is often described as more than simple sleepiness. It can feel like heaviness, reduced stamina, or the sense that everyday tasks suddenly require extra effort. Some people mention that they can still function, but they no longer feel like themselves. Others notice bloating, discomfort after meals, or clothes fitting differently when fluid retention starts to build. Itching can also become a miserable, underappreciated symptom. It sounds small on paper, but persistent itching can disrupt sleep, concentration, and mood in a very real way.
Jaundice creates another layer of experience because it is visible. When the eyes or skin begin turning yellow, people often feel alarmed, embarrassed, or both. Family members notice. Coworkers notice. Everyone becomes an amateur detective. Dark urine and pale stools can be equally unsettling because they are hard to ignore and often signal that something meaningful is going on with bilirubin handling or bile flow.
There is also the lifestyle side of liver health, which can be a major adjustment. Someone diagnosed with MASLD may suddenly be told to think differently about weight, blood sugar, exercise, and long-term cardiovascular risk. Someone with alcohol-related liver disease may face not only medical treatment but also behavioral change, stigma, and difficult conversations at home. A person with viral hepatitis may wrestle with questions about how they were exposed, what happens next, and how much of the future is now tied to lab results and imaging reports.
Caregivers often describe their own version of the journey. They may notice the symptoms before the patient does: increasing forgetfulness, swelling, bruising, changes in sleep, or subtle personality shifts. In advanced liver disease, confusion can be especially hard for families because it changes communication. The person they love may still be there, but not fully clear, not fully steady, not fully themselves in the moment.
On the positive side, many people also experience a strong sense of relief once they finally get a clear diagnosis and a practical plan. Knowing whether the issue is viral, metabolic, autoimmune, medication-related, or scar-based helps replace vague fear with specific next steps. People often do better when they can move from “Something is wrong” to “Here is what we are watching, here is what we are changing, and here is when we follow up.”
That may be the most human part of liver care: progress is often built through small, unglamorous decisions. Keeping appointments. Repeating labs. Adjusting medications. Skipping alcohol. Walking more. Losing some weight. Managing diabetes better. Asking questions. Taking symptoms seriously. The liver may be a biochemical powerhouse, but the real-life experience of protecting it often comes down to consistency, patience, and not waiting too long to get checked.
Final Thoughts
The liver is a powerhouse organ with a complicated job description and a surprisingly quiet personality. It helps digest food, process nutrients, regulate blood chemistry, clear waste, and support the body in hundreds of ways. Because liver disease can be subtle at first, symptoms such as fatigue, nausea, upper abdominal pain, jaundice, dark urine, swelling, itching, or confusion should not be ignored.
Whether the issue is hepatitis, fatty liver disease, alcohol-related injury, fibrosis, cirrhosis, or another condition entirely, early evaluation matters. The sooner liver problems are identified, the better the chance of reducing damage, treating the cause, and protecting long-term health. In short: your liver has been doing a lot for you. Returning the favor is a pretty good idea.





